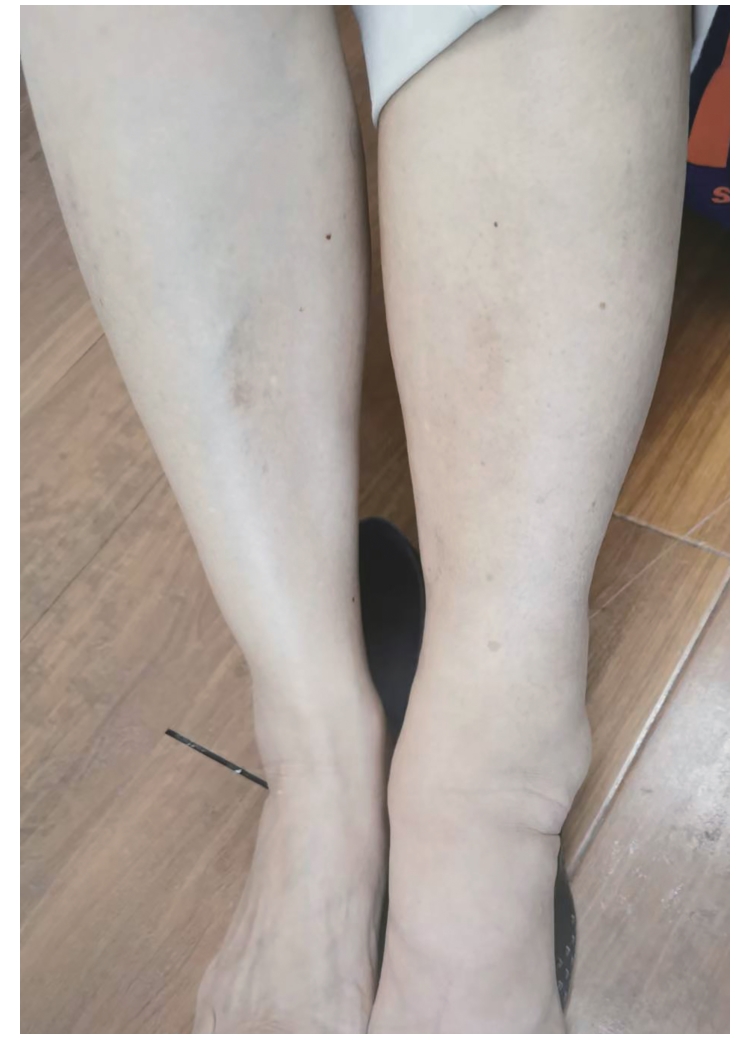
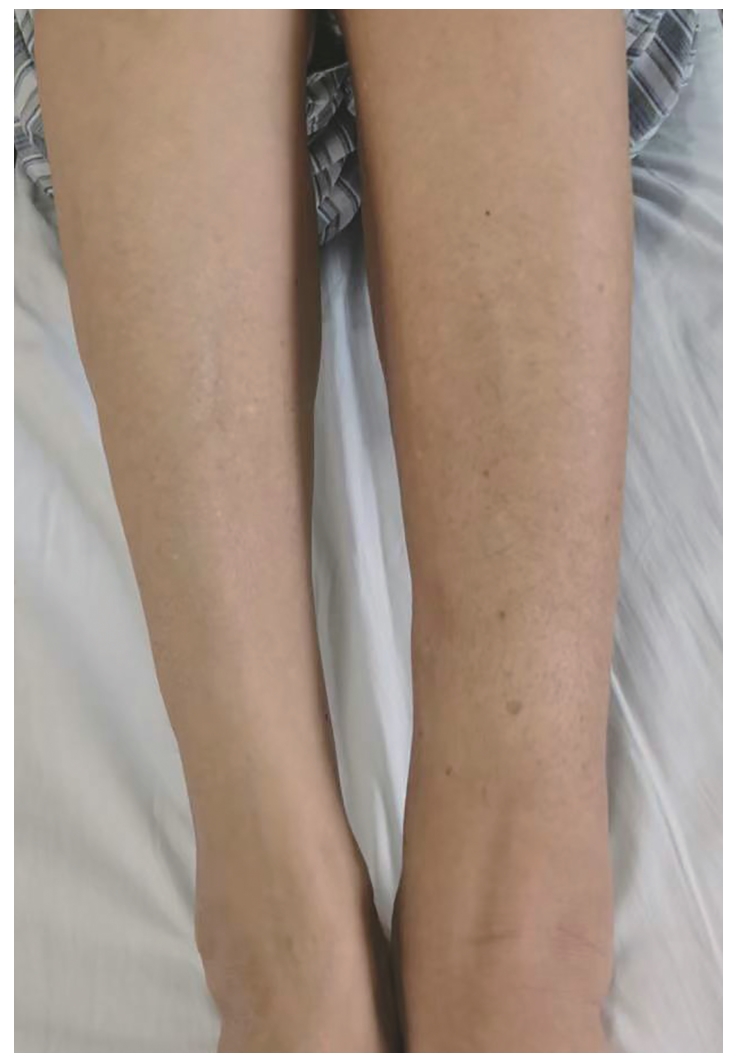
乙型肝炎肝硬化合并路邓葡萄球菌血流感染1例报告
DOI: 10.12449/JCH260221
Hepatitis B cirrhosis comorbid with Staphylococcus lugdunensis bloodstream infection: A case report
-
摘要: 路邓葡萄球菌作为一种凝固酶阴性的葡萄球菌,其毒力和致病性较其他葡萄球菌更强,和金黄色葡萄球菌相当,近年来,相关病例报道逐渐增加,本科收治1例乙型肝炎肝硬化合并路邓葡萄球菌血流感染患者,随访超过2年,分析其临床特性、致病力、侵袭性及相关抗生素应用。Abstract: As a coagulase-negative staphylococcus, Staphylococcus lugdunensis has stronger virulence and pathogenicity than other Staphylococcus bacteria and is comparable to Staphylococcus aureus. In recent years, there has been a gradual increase in the number of related case reports, A patient with hepatitis B cirrhosis and Staphylococcus lugdunensis bloodstream infection was admitted to our department and was followed up for more than 2 years, and the patient was analyzed in terms of clinical features, pathogenicity, invasion, and the application of related antibiotics.
-
Key words:
- Staphylococcus lugdunensis /
- Hepatitis B /
- Liver Cirrhosis /
- Bloodstream Infection
-
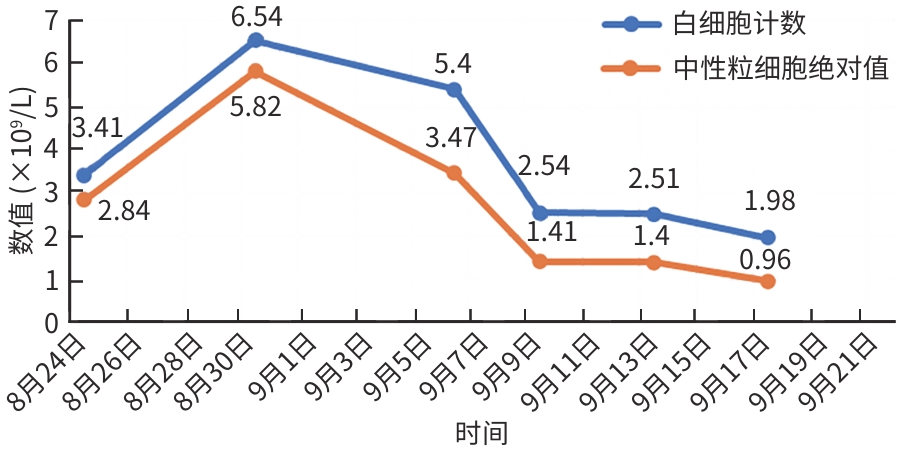
表 1 血常规、炎症指标、最高体温检测及抗生素使用情况
Table 1. Blood routine test, inflammatory markers, maximum body temperature, and antibiotic usage
时间 WBC(×109/L) N%(%) NEUT#(×109/L) CRP(mg/L) 降钙素原(ng/mL) 最高体温(℃) 抗生素使用 2019.11.11 2.86 58.9 1.68 无 无 2020.9.9 2.89 54.7 1.58 无 无 2021.6.26 1.90 55.9 1.06 <0.5 <0.02 无 无 2022.8.24 3.41 83.3 2.84 1.35 <0.02 无 无 2022.8.30 6.54 88.9 5.82 0.52 0.07 39 头孢克洛 2022.9.6 5.40 64.2 3.47 0.63 0.03 无 万古霉素 2022.9.9 2.54 55.5 1.41 0.51 <0.02 无 万古霉素 2022.9.13 2.51 55.7 1.40 1.04 <0.02 无 万古霉素 2022.9.17 1.98 48.6 0.96 <0.5 <0.02 无 万古霉素 注:WBC,白细胞计数;N%,中性粒细胞百分比;NEUT#,中性粒细胞绝对值;CRP,C反应蛋白;空白表示未检测。
表 2 肝肾功能
Table 2. Renal function
时间 ALT(U/L) AST(U/L) LDH(U/L) TBil(μmol/L) SCr(μmol/L) BUN(mmol/L) 2021.8.21 22 27 319 31.0 62 4.90 2022.9.9 14 29 214 29.8 58 4.31 2022.9.13 12 26 199 26.8 58 5.46 2023.10.6 23 30 201 25.5 60 5.31 注:ALT,丙氨酸氨基转移酶;AST,天冬氨酸氨基转移酶;LDH,乳酸脱氢酶;SCr,血肌酐;BUN,尿素。
表 3 路邓葡萄球菌药敏结果
Table 3. Drug sensitivity results of Staphylococcus lugdunensis
抗菌药物 最低抑菌浓度(mg/L) 敏感度 青霉素G ≥0.5 耐药 庆大霉素 ≤0.5 敏感 莫西沙星 ≤0.25 敏感 氯洁霉素 ≤0.12 敏感 达托霉素 0.5 敏感 万古霉素 ≤0.5 敏感 利福平 ≤0.5 敏感 苯唑西林 0.5 敏感 左氧氟沙星 ≤0.12 敏感 红霉素 ≤0.25 敏感 利奈唑胺 1 敏感 替考拉宁 ≤0.5 敏感 替加环素 ≤0.12 敏感 复方新诺明 ≤10 敏感 -
[1] FRENEY J, BRUN Y, BES M, et al. Staphylococcus lugdunensis sp. nov. and Staphylococcus schleiferi sp. nov., Two Species from Human Clinical Specimens[J]. Int J Syst Bacteriol, 1988, 38( 2): 168- 172. DOI: 10.1099/00207713-38-2-168. [2] LU WH, LIU LL, CAO ZL, et al. Adolescent idiopathic scoliosis surgical site infection caused by Staphylococcus lugdunensis: A case report[J]. J Spinal Surg, 2020, 18( 4): 286- 288. DOI: 10.3969/j.issn.1672-2957.2020.04.015.陆伟豪, 刘乐玲, 曹正霖, 等. 路邓葡萄球菌引起青少年特发性脊柱侧凸术后感染1例报告[J]. 脊柱外科杂志, 2020, 18( 4): 286- 288. DOI: 10.3969/j.issn.1672-2957.2020.04.015. [3] BÖCHER S, TØNNING B, SKOV RL, et al. Staphylococcus lugdunensis, a common cause of skin and soft tissue infections in the community[J]. J Clin Microbiol, 2009, 47( 4): 946- 950. DOI: 10.1128/JCM.01024-08. [4] LIU ZJ, SHEN DX. Two cases of bone and joint infections caused by Staphylococcus lugdunensis[J]. Natl Med J China, 2013, 93( 30): 2416. DOI: 10.3760/cma.j.issn.0376-2491.2013.30.022.刘朝军, 沈定霞. 路邓葡萄球菌致骨和关节感染二例[J]. 中华医学杂志, 2013, 93( 30): 2416. DOI: 10.3760/cma.j.issn.0376-2491.2013.30.022. [5] FRANK KL, DEL POZO JL, PATEL R. From clinical microbiology to infection pathogenesis: How daring to be different works for Staphylococcus lugdunensis[J]. Clin Microbiol Rev, 2008, 21( 1): 111- 133. DOI: 10.1128/CMR.00036-07. [6] BECKER K, HEILMANN C, PETERS G. Coagulase-negative staphylococci[J]. Clin Microbiol Rev, 2014, 27( 4): 870- 926. DOI: 10.1128/CMR.00109-13. [7] KLOTCHKO A, WALLACE MR, LICITRA C, et al. Staphylococcus lugdunensis: An emerging pathogen[J]. South Med J, 2011, 104( 7): 509- 514. DOI: 10.1097/SMJ.0b013e31821e91b1. [8] HEILBRONNER S, FOSTER TJ. Staphylococcus lugdunensis: A skin commensal with invasive pathogenic potential[J]. Clin Microbiol Rev, 2021, 34( 2): e00205-20. DOI: 10.1128/CMR.00205-20. [9] DOUIRI N, HANSMANN Y, LEFEBVRE N, et al. Staphylococcus lugdunensis: A virulent pathogen causing bone and joint infections[J]. Clin Microbiol Infect, 2016, 22( 8): 747- 748. DOI: 10.1016/j.cmi.2016.05.031. [10] ZHANG X, CHENG JH, LI X, et al. Clinical characteristics and drug resistance of Staphylococcus lugdunensis infection[J]. Zhejiang Med J, 2023, 45( 20): 2188- 2192, 2201. DOI: 10.12056/j.issn.1006-2785.2023.45.20.2023-936.张霞, 程江豪, 李曦, 等. 路邓葡萄球菌感染的临床特征及耐药性分析[J]. 浙江医学, 2023, 45( 20): 2188- 2192, 2201. DOI: 10.12056/j.issn.1006-2785.2023.45.20.2023-936. [11] LIU YH, MU H, ZHANG JL, et al. Identification, drug resistance spectrum and clinical infection characteristics of Staphylococcus ludden by mass spectrometry[J]. Shandong Med J, 2020, 60( 15): 78- 80. DOI: 10.3969/j.issn.1002-266X.2020.15.021.刘晔华, 穆红, 张坚磊, 等. 路邓葡萄球菌的质谱技术鉴定及耐药谱、临床感染特征分析[J]. 山东医药, 2020, 60( 15): 78- 80. DOI: 10.3969/j.issn.1002-266X.2020.15.021. [12] PARTHASARATHY S, SHAH S, RAJA SAGER A, et al. Staphylococcus lugdunensis: Review of epidemiology, complications, and treatment[J]. Cureus, 2020, 12( 6): e8801. DOI: 10.7759/cureus.8801. [13] LIU CJ, SHEN DX, GUO J, et al. Clinical and microbiological characterization of Staphylococcus lugdunensis isolates obtained from clinical specimens in a hospital in China[J]. BMC Microbiol, 2012, 12: 168. DOI: 10.1186/1471-2180-12-168. [14] HU XY, ZHOU YX. Neonatal catheter-related bloodstream infection caused by methicillin-resistant Staphylococcus lugdunensis: A case report[J]. Chin J Infect Control, 2015, 14( 4): 278- 279. DOI: 10.3969/j.issn.1671-9638.2015.04.018.胡晓艳, 周于新. 耐甲氧西林路邓葡萄球菌致新生儿导管相关血流感染1例[J]. 中国感染控制杂志, 2015, 14( 4): 278- 279. DOI: 10.3969/j.issn.1671-9638.2015.04.018. [15] SHAH NB, OSMON DR, FADEL H, et al. Laboratory and clinical characteristics of Staphylococcus lugdunensis prosthetic joint infections[J]. J Clin Microbiol, 2010, 48( 5): 1600- 1603. DOI: 10.1128/JCM.01769-09. [16] TAN TY, NG SY, HE J. Microbiological characteristics, presumptive identification, and antibiotic susceptibilities of Staphylococcus lugdunensis[J]. J Clin Microbiol, 2008, 46( 7): 2393- 2395. DOI: 10.1128/JCM.00740-08. [17] CUI W, TIAN SS, FENG BE, et al. Identification, drug resistance and clinical infection analysis of Staphylococcus lugdunensis[J/CD]. Chin J Exp Clin Infect Dis Electron Version, 2018, 12( 1): 80- 84. DOI: 10.3877/cma.j.issn.1674-1358.2018.01.016.崔嵬, 田树时, 冯柏娥, 等. 路邓葡萄球菌的鉴定、耐药和临床感染分析[J/CD]. 中华实验和临床感染病杂志(电子版), 2018, 12( 1): 80- 84. DOI: 10.3877/cma.j.issn.1674-1358.2018.01.016. [18] MATAS A, VEIGA A, GABRIEL JP. Brain abscess due to Staphylococcus lugdunensis in the absence of endocarditis or bacteremia[J]. Case Rep Neurol, 2015, 7( 1): 1- 5. DOI: 10.1159/000371441. -



 PDF下载 ( 18288 KB)
PDF下载 ( 18288 KB)

 下载:
下载: