自身免疫性肝病与自身免疫性甲状腺疾病共病的机制及临床特点
DOI: 10.12449/JCH260225
利益冲突声明:本文不存在任何利益冲突。
作者贡献声明:冉应会负责选题,撰写论文;卢维、杨富梅、李小红负责文章审阅,修改论文;朱蓉负责最终版本修订。
The mechanism and clinical characteristics in comorbidity of autoimmune liver diseases and autoimmune thyroid diseases
-
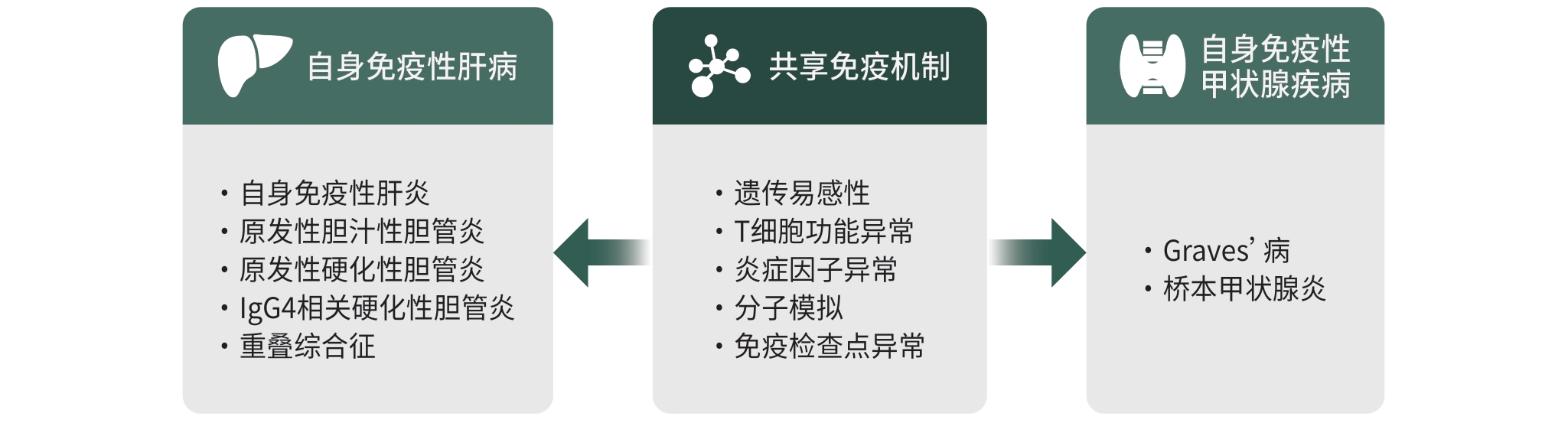
摘要: 自身免疫性肝病(AILD)是一组由免疫系统异常激活引发的慢性肝脏疾病,主要包括自身免疫性肝炎、原发性胆汁性胆管炎、原发性硬化性胆管炎、IgG4相关硬化性胆管炎和重叠综合征。临床研究显示,AILD患者常伴有甲状腺疾病,特别是自身免疫性甲状腺疾病(AITD),如Graves’病和桥本甲状腺炎。本文系统综述了AILD与甲状腺疾病的流行病学关联、潜在的共同发病机制和临床表现重叠特征。通过深入探讨AILD与AITD之间的免疫关联,有望为精准诊疗及未来研究提供理论支持。Abstract: Autoimmune liver diseases (AILD) are a group of chronic liver diseases caused by abnormal activation of the immune system, mainly including autoimmune hepatitis, primary biliary cholangitis, primary sclerosing cholangitis, IgG4-related sclerosing cholangitis, and overlap syndrome. Clinical studies have shown that patients with AILD are often comorbid with thyroid diseases, especially autoimmune thyroid diseases (AITD), such as Graves’ disease and Hashimoto’s thyroiditis. This article systematically reviews the epidemiological association, potential shared pathogenesis, and overlapping features between AILD and thyroid diseases. A deeper understanding of the immunological links between AILD and AITD may provide a theoretical basis for precision medicine and future research.
-
Key words:
- Hepatitis, Autoimmune /
- Thyroid Disease /
- Comorbidity
-
[1] TANAKA A. Autoimmune hepatitis: 2019 update[J]. Gut Liver, 2020, 14( 4): 430- 438. DOI: 10.5009/gnl19261. [2] WANG GQ, TANAKA A, ZHAO H, et al. The Asian Pacific Association for the Study of the Liver clinical practice guidance: The diagnosis and management of patients with autoimmune hepatitis[J]. Hepatol Int, 2021, 15( 2): 223- 257. DOI: 10.1007/s12072-021-10170-1. [3] Korean Association for the Study of the Liver(KASL). KASL clinical practice guidelines for management of autoimmune hepatitis 2022[J]. Clin Mol Hepatol, 2023, 29( 3): 542- 592. DOI: 10.3350/cmh.2023.0087. [4] REAU NS, LAMMERT CS, WEINBERG EM. Autoimmune hepatitis: Current and future therapies[J]. Hepatol Commun, 2024, 8( 6): e0458. DOI: 10.1097/HC9.0000000000000458. [5] MENG ZL, YANG YD. Advances in the treatment of autoimmune hepatitis[J]. J Clin Transl Hepatol, 2024, 12( 10): 878- 885. DOI: 10.14218/JCTH.2024.00193. [6] VERGANI D, MIELI-VERGANI G. Pharmacological management of autoimmune hepatitis[J]. Expert Opin Pharmacother, 2011, 12( 4): 607- 613. DOI: 10.1517/14656566.2011.524206. [7] YOUNOSSI ZM, BERNSTEIN D, SHIFFMAN ML, et al. Diagnosis and management of primary biliary cholangitis[J]. Am J Gastroenterol, 2019, 114( 1): 48- 63. DOI: 10.1038/s41395-018-0390-3. [8] LEVY C, MANNS M, HIRSCHFIELD G. New treatment paradigms in primary biliary cholangitis[J]. Clin Gastroenterol Hepatol, 2023, 21( 8): 2076- 2087. DOI: 10.1016/j.cgh.2023.02.005. [9] TANAKA A. Current understanding of primary biliary cholangitis[J]. Clin Mol Hepatol, 2021, 27( 1): 1- 21. DOI: 10.3350/cmh.2020.0028. [10] SARCOGNATO S, SACCHI D, GRILLO F, et al. Autoimmune biliary diseases: Primary biliary cholangitis and primary sclerosing cholangitis[J]. Pathologica, 2021, 113( 3): 170- 184. DOI: 10.32074/1591-951X-245. [11] JI JG, SUNDQUIST J, SUNDQUIST K. Gender-specific incidence of autoimmune diseases from national registers[J]. J Autoimmun, 2016, 69: 102- 106. DOI: 10.1016/j.jaut.2016.03.003. [12] RONCA V, DAVIES SP, OO YH, et al. The immunological landscape of primary biliary cholangitis: Mechanisms and therapeutic prospects[J]. Hepatology, 2025, 82( 4): 877- 894. DOI: 10.1097/HEP.0000000000001225. [13] BARBA BERNAL R, FERRIGNO B, MEDINA MORALES E, et al. Management of primary biliary cholangitis: Current treatment and future perspectives[J]. Turk J Gastroenterol, 2023, 34( 2): 89- 100. DOI: 10.5152/tjg.2023.22239. [14] HIRSCHFIELD GM, GERSHWIN ME. The immunobiology and pathophysiology of primary biliary cirrhosis[J]. Annu Rev Pathol, 2013, 8: 303- 330. DOI: 10.1146/annurev-pathol-020712-164014. [15] Working Subgroup(English version) for Clinical Practice Guidelines for Primary Biliary Cirrhosis. Guidelines for the management of primary biliary cirrhosis: The Intractable Hepatobiliary Disease Study Group supported by the Ministry of Health, Labour and Welfare of Japan[J]. Hepatol Res, 2014, 44( Suppl S1): 71- 90. DOI: 10.1111/hepr.12270. [16] KARLSEN TH, FOLSERAAS T, THORBURN D, et al. Primary sclerosing cholangitis-a comprehensive review[J]. J Hepatol, 2017, 67( 6): 1298- 1323. DOI: 10.1016/j.jhep.2017.07.022. [17] DYSON JK, BEUERS U, JONES DEJ, et al. Primary sclerosing cholangitis[J]. Lancet, 2018, 391( 10139): 2547- 2559. DOI: 10.1016/S0140-6736(18)30300-3. [18] CANÇADO GGL, HIRSCHFIELD GM. Management of primary sclerosing cholangitis: Current state-of-the-art[J]. Hepatol Commun, 2024, 8( 12): e0590. DOI: 10.1097/HC9.0000000000000590. [19] TANAKA A. IgG4-related sclerosing cholangitis and primary sclerosing cholangitis[J]. Gut Liver, 2019, 13( 3): 300- 307. DOI: 10.5009/gnl18085. [20] LAZARIDIS KN, LARUSSO NF. Primary sclerosing cholangitis[J]. N Engl J Med, 2016, 375( 12): 1161- 1170. DOI: 10.1056/nejmra1506330. [21] National Health Commission of the People’s Republic of China. Guidelines for the diagnosis and treatment of primary sclerosing cholangitis(2025 edition)[J]. J Clin Hepatol, 2025, 41( 8): 1507- 1511. DOI: 10.12449/JCH250806.中华人民共和国国家卫生健康委员会. 原发性硬化性胆管炎诊疗指南(2025 年版)[J]. 临床肝胆病杂志, 2025, 41( 8): 1507- 1511. DOI: 10.12449/JCH250806. [22] KATZ G, STONE JH. Clinical perspectives on IgG4-related disease and its classification[J]. Annu Rev Med, 2022, 73: 545- 562. DOI: 10.1146/annurev-med-050219-034449. [23] UMEHARA H, OKAZAKI K, KAWA S, et al. The 2020 revised comprehensive diagnostic(RCD) criteria for IgG4-RD[J]. Mod Rheumatol, 2021, 31( 3): 529- 533. DOI: 10.1080/14397595.2020.1859710. [24] MARITATI F, PEYRONEL F, VAGLIO A. IgG4-related disease: A clinical perspective[J]. Rheumatology, 2020, 59( Suppl 3): iii123-iii 131. DOI: 10.1093/rheumatology/kez667. [25] SÁNCHEZ-ORO R, ALONSO-MUÑOZ EM, MARTÍ ROMERO L. Review of IgG4-related disease[J]. Gastroenterol Hepatol, 2019, 42( 10): 638- 647. DOI: 10.1016/j.gastrohep.2019.08.009. [26] WALLACE ZS, KATZ G, HERNANDEZ-BARCO YG, et al. Current and future advances in practice: IgG4-related disease[J]. Rheumatol Adv Pract, 2024, 8( 2): rkae020. DOI: 10.1093/rap/rkae020. [27] OHARA H, OKAZAKI K, TSUBOUCHI H, et al. Clinical diagnostic criteria of IgG4-related sclerosing cholangitis 2012[J]. J Hepatobiliary Pancreat Sci, 2012, 19( 5): 536- 542. DOI: 10.1007/s00534-012-0521-y. [28] NAITOH I, NAKAZAWA T. Classification and diagnostic criteria for IgG4-related sclerosing cholangitis[J]. Gut Liver, 2022, 16( 1): 28- 36. DOI: 10.5009/gnl210116. [29] DRAZILOVA S, VESELINY E, LENARTOVA PD, et al. IgG4-related sclerosing cholangitis: Rarely diagnosed, but not a rare disease[J]. Can J Gastroenterol Hepatol, 2021, 2021: 1959832. DOI: 10.1155/2021/1959832. [30] HUGGETT MT, CULVER EL, KUMAR M, et al. Type 1 autoimmune pancreatitis and IgG4-related sclerosing cholangitis is associated with extrapancreatic organ failure, malignancy, and mortality in a prospective UK cohort[J]. Am J Gastroenterol, 2014, 109( 10): 1675- 1683. DOI: 10.1038/ajg.2014.223. [31] KHOURY NC, BIRK JW. A review of IgG4-related sclerosing cholangitis(IgG4-SC)[J]. J Clin Gastroenterol, 2024, 58( 10): 963- 969. DOI: 10.1097/MCG.0000000000001984. [32] ZENG QM, ZHAO LL, WANG CY, et al. Relationship between autoimmune liver disease and autoimmune thyroid disease: A cross-sectional study[J]. Scand J Gastroenterol, 2020, 55( 2): 216- 221. DOI: 10.1080/00365521.2019.1710766. [33] TAKAHASHI A, ARINAGA-HINO T, OHIRA H, et al. Autoimmune hepatitis in Japan: Trends in a nationwide survey[J]. J Gastroenterol, 2017, 52( 5): 631- 640. DOI: 10.1007/s00535-016-1267-0. [34] KHOURY T, KADAH A, MARI A, et al. Thyroid dysfunction is prevalent in autoimmune hepatitis: A case control study[J]. Isr Med Assoc J, 2020, 22( 2): 100- 103. [35] LEE YJ, SUNG JY, KIM SH, et al. A case of Hashimoto’s thyroiditis accompanied by autoimmune hepatitis diagnosed with liver biopsy[J]. J Korean Endocr Soc, 2009, 24( 4): 287. DOI: 10.3803/jkes.2009.24.4.287. [36] MANEVSKA N, STOJKOVSKA N, TASHEVA L, et al. Autoimmune Hashimoto thyroiditis with concomitant autoimmune hepatitis[J]. Arch Pub Health, 2022, 14( 1): 151- 156. DOI: 10.3889/aph.2022.6042 [37] LONGHI MS, MA Y, MITRY RR, et al. Effect of CD4+ CD25+ regulatory T-cells on CD8 T-cell function in patients with autoimmune hepatitis[J]. J Autoimmun, 2005, 25( 1): 63- 71. DOI: 10.1016/j.jaut.2005.05.001. [38] HOSSEN MM, MA YM, YIN ZH, et al. Current understanding of CTLA-4: From mechanism to autoimmune diseases[J]. Front Immunol, 2023, 14: 1198365. DOI: 10.3389/fimmu.2023.1198365. [39] HOSSEINI A, GHARIBI T, MAROFI F, et al. CTLA-4: From mechanism to autoimmune therapy[J]. Int Immunopharmacol, 2020, 80: 106221. DOI: 10.1016/j.intimp.2020.106221. [40] FRANCISCO LM, SAGE PT, SHARPE AH. The PD-1 pathway in tolerance and autoimmunity[J]. Immunol Rev, 2010, 236: 219- 242. DOI: 10.1111/j.1600-065X.2010.00923.x. [41] CURNOCK AP, BOSSI G, KUMARAN J, et al. Cell-targeted PD-1 agonists that mimic PD-L1 are potent T cell inhibitors[J]. JCI Insight, 2021, 6( 20): e152468. DOI: 10.1172/jci.insight.152468. [42] CHEN RY, ZHU Y, SHEN YY, et al. The role of PD-1 signaling in health and immune-related diseases[J]. Front Immunol, 2023, 14: 1163633. DOI: 10.3389/fimmu.2023.1163633. [43] LIVZAN MA, GAUS OV, GAVRILENKO DA. Manifest hyperthyroidism in patient with autoimmune hepatitis(clinical observation)[J]. Medicinskij Alfavit, 2021( 35): 52- 56. DOI: 10.33667/2078-5631-2021-35-52-56. [44] ZHENG MF, CUI SY, ZHANG W, et al. Graves’ disease overlapping with chronic hepatitis B and methimazole-induced liver injury and autoimmune hepatitis: A case report[J]. BMC Gastroenterol, 2022, 22( 1): 59. DOI: 10.1186/s12876-022-02133-z. [45] RANA S, AHMED Z, SALGIA R, et al. Successful management of patients with co-existent Graves’ disease and autoimmune hepatitis[J]. Cureus, 2019, 11( 5): e4647. DOI: 10.7759/cureus.4647. [46] LIANG Y, LI J, ZHANG ZY, et al. Extrahepatic conditions of primary biliary cholangitis: A systematic review and meta-analysis of prevalence and risk[J]. Clin Res Hepatol Gastroenterol, 2024, 48( 5): 102321. DOI: 10.1016/j.clinre.2024.102321. [47] FLOREANI A, MANGINI C, REIG A, et al. Thyroid dysfunction in primary biliary cholangitis: A comparative study at two European centers[J]. Am J Gastroenterol, 2017, 112( 1): 114- 119. DOI: 10.1038/ajg.2016.479. [48] GHOZZI M, MANKAI A, CHEDLY Z, et al. Frequency of antithyroid antibodies in patients with primary biliary cholangitis[J]. Lab Med, 2024, 55( 3): 304- 309. DOI: 10.1093/labmed/lmad080. [49] FLOREANI A, FRANCESCHET I, CAZZAGON N, et al. Extrahepatic autoimmune conditions associated with primary biliary cirrhosis[J]. Clin Rev Allergy Immunol, 2015, 48( 2-3): 192- 197. DOI: 10.1007/s12016-014-8427-x. [50] MA G, YANG JQ, WANG XG, et al. Dissecting causal relationships between primary biliary cholangitis and extrahepatic autoimmune diseases based on Mendelian randomization[J]. Sci Rep, 2024, 14( 1): 11528. DOI: 10.1038/s41598-024-62509-x. [51] KUŚ A, ARŁUKOWICZ-GRABOWSKA M, SZYMAŃSKI K, et al. Genetic risk factors for autoimmune thyroid disease might affect the susceptibility to and modulate the progression of primary biliary cholangitis[J]. J Gastrointestin Liver Dis, 2017, 26( 3): 245- 252. DOI: 10.15403/jgld.2014.1121.263.kus. [52] PAMFIL C, CANDREA E, BERKI E, et al. Primary biliary cirrhosis: Autoimmune hepatitis overlap syndrome associated with dermatomyositis, autoimmune thyroiditis and antiphospholipid syndrome[J]. J Gastrointestin Liver Dis, 2015, 24( 1): 101- 104. DOI: 10.15403/jgld.2014.1121.cpa. [53] CHEN S, LI MQ, DUAN WJ, et al. Concomitant extrahepatic autoimmune diseases do not compromise the long-term outcomes of primary biliary cholangitis[J]. Hepatobiliary Pancreat Dis Int, 2022, 21( 6): 577- 582. DOI: 10.1016/j.hbpd.2022.05.009. [54] KHAN AA, ATA F, AZIZ A, et al. Clinical characteristics and outcomes of patients with antithyroid drug-related liver injury[J]. J Endocr Soc, 2023, 8( 1): bvad133. DOI: 10.1210/jendso/bvad133. [55] FAISAL A. Understanding fatigue and pruritus in primary biliary cholangitis[J]. Clin Liver Dis, 2024, 23( 1): e0216. DOI: 10.1097/CLD.0000000000000216. [56] ZHANG WH, LANG R. Genetic link between primary sclerosing cholangitis and thyroid dysfunction: A bidirectional two-sample Mendelian randomization study[J]. Front Immunol, 2023, 14: 1276459. DOI: 10.3389/fimmu.2023.1276459. [57] HUANG P, HOU YQ, ZOU YX, et al. The causal effects of primary biliary cholangitis on thyroid dysfunction: A two-sample mendelian randomization study[J]. Front Genet, 2021, 12: 791778. DOI: 10.3389/fgene.2021.791778. [58] LAMBERTS LE, JANSE M, HAAGSMA EB, et al. Immune-mediated diseases in primary sclerosing cholangitis[J]. Dig Liver Dis, 2011, 43( 10): 802- 806. DOI: 10.1016/j.dld.2011.05.009. [59] ALEKSANDROVA EA, BURNEVICH EZ, ARION EA. Systemic manifestations of primary sclerosing cholangitis[J]. Klin Med, 2013, 91( 4): 38- 42. [60] HOV JR, BOBERG KM, KARLSEN TH. Autoantibodies in primary sclerosing cholangitis[J]. World J Gastroenterol, 2008, 14( 24): 3781- 3791. DOI: 10.3748/wjg.14.3781. [61] ANGULO P, PETER JB, GERSHWIN ME, et al. Serum autoantibodies in patients with primary sclerosing cholangitis[J]. J Hepatol, 2000, 32( 2): 182- 187. DOI: 10.1016/s0168-8278(00)80061-6. [62] WATANABE T, MARUYAMA M, ITO T, et al. Clinical features of a new disease concept, IgG4-related thyroiditis[J]. Scand J Rheumatol, 2013, 42( 4): 325- 330. DOI: 10.3109/03009742.2012.761281. [63] IOACHIM D, PUBLIK MA, TERZEA D, et al. IgG4-mediated sclerosing riedel thyroiditis: A multidisciplinary case study and literature review[J]. Int J Mol Sci, 2025, 26( 16): 7786. DOI: 10.3390/ijms26167786. [64] CZARNYWOJTEK A, PIETROŃCZYK K, THOMPSON LDR, et al. IgG4-related sclerosing thyroiditis(Riedel-Struma): A review of clinicopathological features and management[J]. Virchows Arch, 2023, 483( 2): 133- 144. DOI: 10.1007/s00428-023-03561-2. -



 PDF下载 ( 683 KB)
PDF下载 ( 683 KB)

 下载:
下载:


