雌激素缺乏通过肠道屏障影响自身免疫性肝炎的作用机制
DOI: 10.12449/JCH260226
Mechanism of action of estrogen deficiency in autoimmune hepatitis via the intestinal barrier
-
摘要: 自身免疫性肝炎(AIH)是一种由免疫介导的慢性肝脏炎性疾病,其发病机制尚未完全阐明,肠道屏障功能障碍被认为是潜在的重要环节。同时,AIH的发病率与严重程度存在性别及年龄差异,提示激素可能参与调控。基于此,本文围绕雌激素、肠道屏障与免疫稳态的关联,系统综述了雌激素缺乏破坏肠道屏障稳态的证据,并进一步归纳了雌激素通过肠道屏障调控AIH发生发展的潜在机制。此外,本文提出雌激素干预的“时间窗”理论可能同样适用于AIH,为AIH的早期预防与个体化治疗提供了新思路。Abstract: Autoimmune hepatitis (AIH) is an immune-mediated chronic liver inflammatory disease with unknown pathogenesis, and intestinal barrier dysfunction is considered an important factor. Meanwhile, there are sex and age differences in the incidence rate of AIH, suggesting that hormone may be involved in regulation. On this basis, this article focuses on the association between estrogen, intestinal barrier, and immune homeostasis, systematically reviews the evidence that estrogen deficiency disrupts intestinal barrier homeostasis, and further summarizes the potential mechanism of estrogen in regulating the development and progression of AIH via intestinal barrier.
-
Key words:
- Estrogens /
- Intestinal Barrier Function /
- Hepatitis, Autoimmune
-
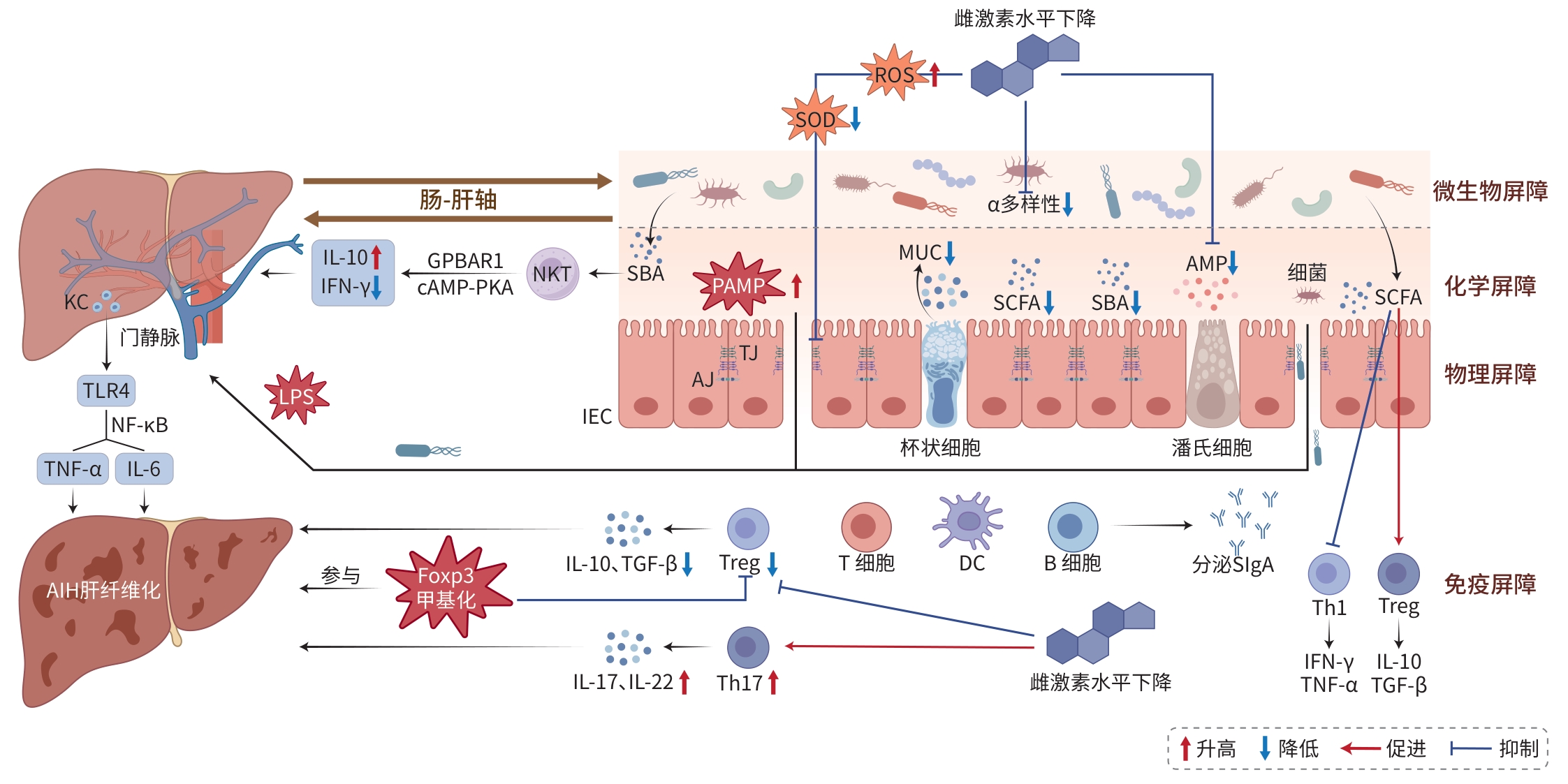
注: AJ,黏附连接;AMP,抗菌肽;cAMP-PKA,环磷酸腺苷-蛋白激酶A信号通路;DC,树突状细胞;GPBAR1受体,G蛋白偶联胆汁酸受体1;IEC,肠上皮细胞;KC,肝巨噬细胞;LPS,脂多糖;MUC,黏蛋白;PAMP,病原体相关分子模式;ROS,活性氧;SlgA,分泌型免疫球蛋白A;SCFA,短链脂肪酸;SBA,次级胆汁酸;SOD,超氧化物歧化酶;TJ,紧密连接;Treg,调节性T细胞;Th17,辅助性T细胞17;TLR4,Toll样受体4;TNF-α,肿瘤坏死因子-α;IL,白细胞介素;AIH,自身免疫性肝炎;FoxP3,叉头框蛋白P3;TGF-β,转化生长因子-β;IFN-γ,γ干扰素。
图 1 雌激素缺乏调控肠道屏障影响AIH的作用机制图
Figure 1. TMechanism Underlying Estrogen Deficiency-Induced AIH via Gut Barrier Dysfunction
-
[1] WANG YY, ZHU L, DING XT. Clinical misdiagnosis of autoimmune hepatitis[J]. Clin Misdiagn Misther, 2024, 37( 2): 25- 28. DOI: 10.3969/j.issn.1002-3429.2024.02.005.王媛媛, 朱丽, 丁秀婷. 自身免疫性肝炎临床误诊分析[J]. 临床误诊误治, 2024, 37( 2): 25- 28. DOI: 10.3969/j.issn.1002-3429.2024.02.005. [2] Chinese Society of Hepatology, Chinese Medical Association. Guidelines on the diagnosis and management of autoimmune hepatitis(2021)[J]. J Clin Hepatol, 2022, 38( 1): 42- 49. DOI: 10.3969/j.issn.1001-5256.2022.01.008.中华医学会肝病学分会. 自身免疫性肝炎诊断和治疗指南(2021)[J]. 临床肝胆病杂志, 2022, 38( 1): 42- 49. DOI: 10.3969/j.issn.1001-5256.2022.01.008. [3] SUCHER E, SUCHER R, GRADISTANAC T, et al. Autoimmune hepatitis-immunologically triggered liver pathogenesis-diagnostic and therapeutic strategies[J]. J Immunol Res, 2019, 2019: 9437043. DOI: 10.1155/2019/9437043. [4] HENEGHAN MA, LOHSE AW. Update in clinical science: Autoimmune hepatitis[J]. J Hepatol, 2025, 82( 5): 926- 937. DOI: 10.1016/j.jhep.2024.12.041. [5] DONET JA, PERLINI EF, GILINSKY D, et al. FRI-393 impact of gender on clinical presentation, response to treatment, and long-term outcomes in an ethnically diverse population of patients with autoimmune hepatitis[J]. J Hepatol, 2016, 64( 2): S439. DOI: 10.1016/S0168-8278(16)00722-4. [6] WU HL, SHI HB, LIU YM, et al. Clinical features and prognosis of autoimmune hepatitis patients with different sexes[J]. J Clin Hepatol, 2021, 37( 7): 1636- 1643. DOI: 10.3969/j.issn.1001-5256.2021.07.031.伍慧丽, 时红波, 刘燕敏, 等. 性别差异对自身免疫性肝炎患者临床特征及预后的影响[J]. 临床肝胆病杂志, 2021, 37( 7): 1636- 1643. DOI: 10.3969/j.issn.1001-5256.2021.07.031. [7] ZHANG QJ, YAN JY. Pregnancy complicated with autoimmune hepatitis[J]. J Pract Obstet Gynecol, 2021, 37( 8): 575- 578.张勤建, 颜建英. 妊娠合并自身免疫性肝炎[J]. 实用妇产科杂志, 2021, 37( 8): 575- 578. [8] KIM BH, CHOI HY, KI M, et al. Population-based prevalence, incidence, and disease burden of autoimmune hepatitis in South Korea[J]. PLoS One, 2017, 12( 8): e0182391. DOI: 10.1371/journal.pone.0182391. [9] KASARINAITE A, SINTON M, SAUNDERS PTK, et al. The influence of sex hormones in liver function and disease[J]. Cells, 2023, 12( 12): 1604. DOI: 10.3390/cells12121604. [10] WANG HQ, SUN DS, WANG H, et al. Mechanism of action of sex hormones in regulating T cell-mediated autoimmune hepatitis: A study based on the phenomenon of female bias[J]. J Clin Hepatol, 2025, 41( 4): 742- 747. DOI: 10.12449/JCH250421.王海强, 孙大沙, 王晗, 等. 基于女性偏倚现象探讨性激素调控T淋巴细胞介导自身免疫性肝炎的作用机制[J]. 临床肝胆病杂志, 2025, 41( 4): 742- 747. DOI: 10.12449/JCH250421. [11] SUN C, ZHU DZ, ZHU Q, et al. The significance of gut microbiota in the etiology of autoimmune hepatitis: A narrative review[J]. Front Cell Infect Microbiol, 2024, 14: 1337223. DOI: 10.3389/fcimb.2024.1337223. [12] AI J, DUAN XY, CHEN P. Research progress of intestinal flora in the repair of intestinal barrier injury in ulcerative colitis[J]. J Med Res, 2025, 54( 2): 193- 195, 214. DOI: 10.11969/j.issn.1673-548X.2025.02.031.艾静, 段晓燕, 陈平. 肠道菌群在溃疡性结肠炎肠道屏障损伤修复中的研究进展[J]. 医学研究杂志, 2025, 54( 2): 193- 195, 214. DOI: 10.11969/j.issn.1673-548X.2025.02.031. [13] ALBILLOS A, de GOTTARDI A, RESCIGNO M. The gut-liver axis in liver disease: Pathophysiological basis for therapy[J]. J Hepatol, 2020, 72( 3): 558- 577. DOI: 10.1016/j.jhep.2019.10.003. [14] ZHANG HX. The role and mechanism of leaky gut in the pathogenesis of autoimmune hepatitis[D]. Tianjin: Tianjin Medical University, 2021. DOI: 10.27366/d.cnki.gtyku.2021.000039.张红霞. 肠黏膜屏障破坏在自身免疫性肝炎发病中的作用和机制[D]. 天津: 天津医科大学, 2021. DOI: 10.27366/d.cnki.gtyku.2021.000039. [15] PLAZA-DÍAZ J, SOLÍS-URRA P, RODRÍGUEZ-RODRÍGUEZ F, et al. The gut barrier, intestinal microbiota, and liver disease: Molecular mechanisms and strategies to manage[J]. Int J Mol Sci, 2020, 21( 21): 8351. DOI: 10.3390/ijms21218351. [16] TAO QQ, OUYANG JX, LI GH, et al. Advances in silymarin modulating intestinal barrier function in poultry[J]. China Feed, 2024( 14): 1- 4. DOI: 10.15906/j.cnki.cn11-2975/s.20241401.陶清清, 欧阳经鑫, 黎观红, 等. 水飞蓟素调控家禽肠道屏障功能研究进展[J]. 中国饲料, 2024( 14): 1- 4. DOI: 10.15906/j.cnki.cn11-2975/s.20241401. [17] JOHANSSON MEV, PHILLIPSON M, PETERSSON J, et al. The inner of the two Muc2 mucin-dependent mucus layers in colon is devoid of bacteria[J]. Proc Natl Acad Sci USA, 2008, 105( 39): 15064- 15069. DOI: 10.1073/pnas.0803124105. [18] AN J, LIU YQ, WANG YQ, et al. The role of intestinal mucosal barrier in autoimmune disease: A potential target[J]. Front Immunol, 2022, 13: 871713. DOI: 10.3389/fimmu.2022.871713. [19] YANG H, LIU QQ, LIU HX, et al. Berberine alleviates concanavalin A-induced autoimmune hepatitis in mice by modulating the gut microbiota[J]. Hepatol Commun, 2024, 8( 4): e0381. DOI: 10.1097/HC9.0000000000000381. [20] ZHANG W, CHEN SL, TIAN YK, et al. Progress on effect of probiotics on porcine intestinal barrier function[J]. Prog Vet Med, 2025, 46( 2): 125- 129. DOI: 10.16437/j.cnki.1007-5038.2025.02.015.张伟, 陈穗莲, 田永宽, 等. 益生菌对猪肠道屏障功能的影响研究概况[J]. 动物医学进展, 2025, 46( 2): 125- 129. DOI: 10.16437/j.cnki.1007-5038.2025.02.015. [21] KUO WT, ODENWALD MA, TURNER JR, et al. Tight junction proteins occludin and ZO-1 as regulators of epithelial proliferation and survival[J]. Ann N Y Acad Sci, 2022, 1514( 1): 21- 33. DOI: 10.1111/nyas.14798. [22] WU JL, ZOU JY, HU ED, et al. Sodium butyrate ameliorates S100/FCA-induced autoimmune hepatitis through regulation of intestinal tight junction and toll-like receptor 4 signaling pathway[J]. Immunol Lett, 2017, 190: 169- 176. DOI: 10.1016/j.imlet.2017.08.005. [23] JANDHYALA SM, TALUKDAR R, SUBRAMANYAM C, et al. Role of the normal gut microbiota[J]. World J Gastroenterol, 2015, 21( 29): 8787- 8803. DOI: 10.3748/wjg.v21.i29.8787. [24] WEI YR, LI YM, YAN L, et al. Alterations of gut microbiome in autoimmune hepatitis[J]. Gut, 2020, 69( 3): 569- 577. DOI: 10.1136/gutjnl-2018-317836. [25] CHENG ZL, YANG L, CHU HK. The gut microbiota: A novel player in autoimmune hepatitis[J]. Front Cell Infect Microbiol, 2022, 12: 947382. DOI: 10.3389/fcimb.2022.947382. [26] LEE J, PEESH P, QUAICOE V, et al. Estradiol mediates colonic epithelial protection in aged mice after stroke and is associated with shifts in the gut microbiome[J]. Gut Microbes, 2023, 15( 2): 2271629. DOI: 10.1080/19490976.2023.2271629. [27] LIWINSKI T, HEINEMANN M, SCHRAMM C. The intestinal and biliary microbiome in autoimmune liver disease-current evidence and concepts[J]. Semin Immunopathol, 2022, 44( 4): 485- 507. DOI: 10.1007/s00281-022-00936-6. [28] RIZZETTO L, FAVA F, TUOHY KM, et al. Connecting the immune system, systemic chronic inflammation and the gut microbiome: The role of sex[J]. J Autoimmun, 2018, 92: 12- 34. DOI: 10.1016/j.jaut.2018.05.008. [29] JIN Y, GAO XY, ZHAO J, et al. Estrogen deficiency aggravates fluoride-induced small intestinal mucosa damage and junctional complexes proteins expression disorder in rats[J]. Ecotoxicol Environ Saf, 2022, 246: 114181. DOI: 10.1016/j.ecoenv.2022.114181. [30] QI XY, YUN CY, PANG YL, et al. The impact of the gut microbiota on the reproductive and metabolic endocrine system[J]. Gut Microbes, 2021, 13( 1): 1894070. DOI: 10.1080/19490976.2021.1894070. [31] FLORES R, SHI JX, FUHRMAN B, et al. Fecal microbial determinants of fecal and systemic estrogens and estrogen metabolites: A cross-sectional study[J]. J Transl Med, 2012, 10: 253. DOI: 10.1186/1479-5876-10-253. [32] MAYNERIS-PERXACHS J, ARNORIAGA-RODRÍGUEZ M, LUQUE-CÓRDOBA D, et al. Gut microbiota steroid sexual dimorphism and its impact on gonadal steroids: Influences of obesity and menopausal status[J]. Microbiome, 2020, 8( 1): 136. DOI: 10.1186/s40168-020-00913-x. [33] MOHAMMAD I, STARSKAIA I, NAGY T, et al. Estrogen receptor α contributes to T cell-mediated autoimmune inflammation by promoting T cell activation and proliferation[J]. Sci Signal, 2018, 11( 526): eaap9415. DOI: 10.1126/scisignal.aap9415. [34] GUO MY, LIU HJ, YU YT, et al. Lactobacillus rhamnosus GG ameliorates osteoporosis in ovariectomized rats by regulating the Th17/Treg balance and gut microbiota structure[J]. Gut Microbes, 2023, 15( 1): 2190304. DOI: 10.1080/19490976.2023.2190304. [35] LIN R, ZHOU L, ZHANG J, et al. Abnormal intestinal permeability and microbiota in patients with autoimmune hepatitis[J]. Int J Clin Exp Pathol, 2015, 8( 5): 5153- 5160. [36] PRADERE JP, TROEGER J, DAPITO D, et al. Toll-like receptor 4 and hepatic fibrogenesis[J]. Semin Liver Dis, 2010, 30( 3): 232- 244. DOI: 10.1055/s-0030-1255353. [37] KANG YB, KUANG XY, YAN H, et al. A novel synbiotic alleviates autoimmune hepatitis by modulating the gut microbiota-liver axis and inhibiting the hepatic TLR4/NF-κB/NLRP3 signaling pathway[J]. mSystems, 2023, 8( 2): e01127-22. DOI: 10.1128/msystems.01127-22. [38] JIA XY, ZHENG LW, YUAN Q, et al. Intestinal microbiota: The new target for the treatment of postmenopausal osteoporosis[J]. Chin J Osteoporos, 2017, 23( 3): 392- 401. DOI: 10.3969/j.issn.1006-7108.2017.03.023.贾小玥, 郑黎薇, 袁泉, 等. 肠道菌群: 绝经后骨质疏松防治新靶点[J]. 中国骨质疏松杂志, 2017, 23( 3): 392- 401. DOI: 10.3969/j.issn.1006-7108.2017.03.023. [39] MIZUNO M, NOTO D, KAGA N, et al. The dual role of short fatty acid chains in the pathogenesis of autoimmune disease models[J]. PLoS One, 2017, 12( 2): e0173032. DOI: 10.1371/journal.pone.0173032. [40] BIAGIOLI M, CARINO A, FIORUCCI C, et al. GPBAR1 functions as gatekeeper for liver NKT cells and provides counterregulatory signals in mouse models of immune-mediated hepatitis[J]. Cell Mol Gastroenterol Hepatol, 2019, 8( 3): 447- 473. DOI: 10.1016/j.jcmgh.2019.06.003. [41] ZHAO L, TANG YL, YOU ZR, et al. Interleukin-17 contributes to the pathogenesis of autoimmune hepatitis through inducing hepatic interleukin-6 expression[J]. PLoS One, 2011, 6( 4): e18909. DOI: 10.1371/journal.pone.0018909. [42] WANG LF, ZHU JX, LIU GW. Research progress on the influence of intestinal microorganisms, Th17 cells and Treg cells on autoimmune hepatitis[J]. Chin J Integr Tradit West Med Liver Dis, 2024, 34( 10): 948- 952. DOI: 10.3969/j.issn.1005-0264.2024.010.019.王莉芬, 朱金霞, 刘光伟. 肠道微生物、Th17细胞和Treg细胞影响自身免疫性肝炎的研究进展[J]. 中西医结合肝病杂志, 2024, 34( 10): 948- 952. DOI: 10.3969/j.issn.1005-0264.2024.010.019. [43] POLANCZYK MJ, HOPKE C, HUAN JY, et al. Enhanced FoxP3 expression and Treg cell function in pregnant and estrogen-treated mice[J]. J Neuroimmunol, 2005, 170( 1-2): 85- 92. DOI: 10.1016/j.jneuroim.2005.08.023. [44] YU YY, SU TT, YANG RM, et al. Exploration of molecular mechanism of Jianpi Yanggan Decoction in treating autoimmune hepatitis based on Th17/Treg axis[J]. J Changchun Univ Chin Med, 2024, 40( 12): 1330- 1334. DOI: 10.13463/j.cnki.cczyy.2024.12.008.于盈盈, 孙婷婷, 杨润萌, 等. 基于Th17/Treg轴探讨健脾养肝汤治疗自身免疫性肝炎的分子机制[J]. 长春中医药大学学报, 2024, 40( 12): 1330- 1334. DOI: 10.13463/j.cnki.cczyy.2024.12.008. [45] LYU TT. Diethylstilbestrol inhibit conA-induced acute autoimmune hepatitis in mouse[D]. Guangzhou: Southern Medical University, 2013. DOI: 10.7666/d.Y2405880.吕廷廷. 己烯雌酚抑制刀豆蛋白A诱导的小鼠急性自身免疫性肝炎[D]. 广州: 南方医科大学, 2013. DOI: 10.7666/d.Y2405880. [46] ZHANG YW, WANG L, QIU SL, et al. Effect of high concentration estradiol on acute autoimmune hepatitis induced by ConA[J]. J Sun Yat Sen Univ Med Sci, 2021, 42( 2): 185- 192. DOI: 10.13471/j.cnki.j.sun.yat-sen.univ(med.sci).2021.0025.张译文, 汪黎, 邱素苈, 等. 高浓度雌二醇对刀豆蛋白A诱导小鼠急性自身免疫性肝炎的影响[J]. 中山大学学报(医学科学版), 2021, 42( 2): 185- 192. DOI: 10.13471/j.cnki.j.sun.yat-sen.univ(med.sci).2021.0025. [47] ZHANG SQ, YANG CX. Menopause and cardiovascular disease:critical window period for early intervention[J]. Chin J Mult Organ Dis Elder, 2022, 21( 5): 393- 396. DOI: 10.11915/j.issn.1671-5403.2022.05.085.张思旗, 杨春晓. 绝经期与心血管疾病早期干预的时间窗[J]. 中华老年多器官疾病杂志, 2022, 21( 5): 393- 396. DOI: 10.11915/j.issn.1671-5403.2022.05.085. [48] ZHAO CL, ZHAO WX. Influence of estrogen deficiency on metabolic associated fatty liver disease in postmenopausal women[J]. J Clin Hepatol, 2021, 37( 7): 1708- 1712. DOI: 10.3969/j.issn.1001-5256.2021.07.049.赵晨露, 赵文霞. 雌激素缺乏对绝经后女性非酒精性脂肪性肝病的影响[J]. 临床肝胆病杂志, 2021, 37( 7): 1708- 1712. DOI: 10.3969/j.issn.1001-5256.2021.07.049. -



 PDF下载 ( 994 KB)
PDF下载 ( 994 KB)

 下载:
下载:


