肝豆状核变性患者脂代谢紊乱的临床表型与致病机制
DOI: 10.12449/JCH260304
利益冲突声明:本文不存在任何利益冲突。
作者贡献声明:高东静、王睿欣负责文献查阅,初稿写作,机制图绘制;李新华负责设计论文框架和思路,指导撰写、修改文章及定稿。
Clinical phenotypes and pathogenic mechanisms of Wilson disease with lipid metabolism disorders
-
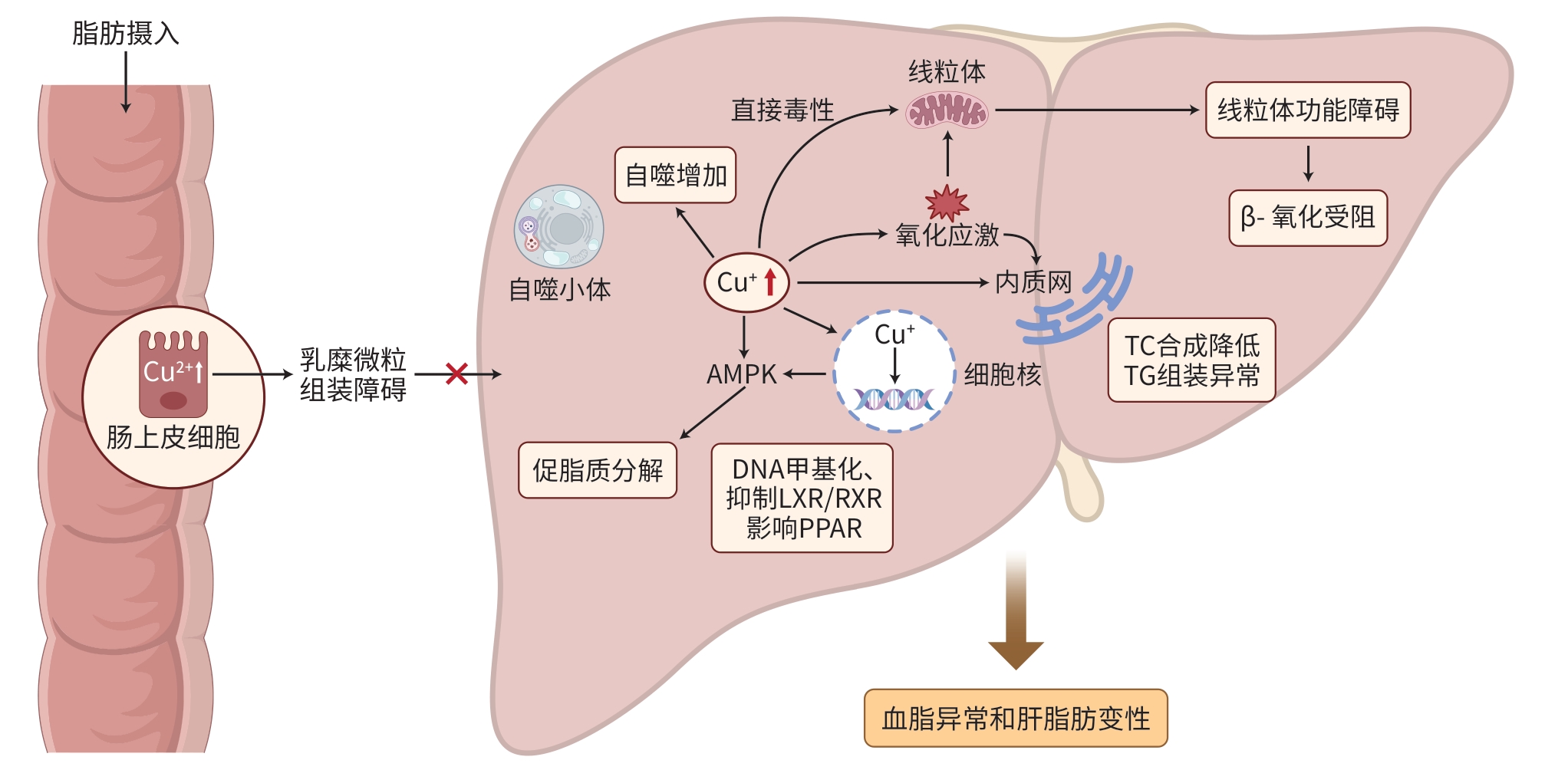
摘要: 肝豆状核变性是一种遗传性铜代谢障碍疾病,其特征是铜在肝脏和大脑等组织中异常蓄积,导致严重的肝脏与神经系统损害。该病常伴随脂代谢异常,其机制探索日益受到关注。本文介绍了肝豆状核变性患者脂代谢紊乱的临床特征,阐述了患者血清脂质水平变化与肝脂肪变性的研究进展,分析了铜与脂代谢相互作用的潜在机制,并总结了脂代谢相关分子在疾病诊断与临床评估中的意义。临床实践中应重视对肝豆状核变性患者脂代谢指标的监测与评估,以期促进该病的综合管理并改善患者预后。Abstract: Wilson disease (WD) is a hereditary disorder of copper metabolism characterized by abnormal copper accumulation in tissues, including the liver and brain, which leads to severe hepatic and neurological damage. This disease is often accompanied by lipid metabolism abnormalities, and the exploration of related mechanisms has attracted increasing attention. This article introduces the clinical features of lipid metabolism disorders in WD patients, summarizes the research advances in the serum levels of lipids and hepatic steatosis, analyzes the potential mechanisms of the interaction between copper and lipid metabolism, and highlights the significance of lipid-related molecules in disease diagnosis and clinical evaluation. In clinical practice, the monitoring and assessment of lipid metabolism parameters should be taken seriously in patients with WD, in order to promote comprehensive disease management and improve the prognosis of patients.
-
[1] SCHILSKY ML, ROBERTS EA, BRONSTEIN JM, et al. A multidisciplinary approach to the diagnosis and management of Wilson disease: 2022 Practice Guidance on Wilson disease from the American Association for the Study of Liver Diseases[J]. Hepatology, 2025, 82( 3): E41- E90. DOI: 10.1002/hep.32801. [2] CZŁONKOWSKA A, LITWIN T, DUSEK P, et al. Wilson disease[J]. Nat Rev Dis Primers, 2018, 4: 21. DOI: 10.1038/s41572-018-0018-3. [3] SAUER SW, MERLE U, OPP S, et al. Severe dysfunction of respiratory chain and cholesterol metabolism in Atp7b(-/-) mice as a model for Wilson disease[J]. Biochim Biophys Acta, 2011, 1812( 12): 1607- 1615. DOI: 10.1016/j.bbadis.2011.08.011. [4] HUSTER D, PURNAT TD, BURKHEAD JL, et al. High copper selectively alters lipid metabolism and cell cycle machinery in the mouse model of Wilson disease[J]. J Biol Chem, 2007, 282( 11): 8343- 8355. DOI: 10.1074/jbc.M607496200. [5] RALLE M, HUSTER D, VOGT S, et al. Wilson disease at a single cell level: Intracellular copper trafficking activates compartment-specific responses in hepatocytes[J]. J Biol Chem, 2010, 285( 40): 30875- 30883. DOI: 10.1074/jbc.M110.114447. [6] LEVY E, BRUNET S, ALVAREZ F, et al. Abnormal hepatobiliary and circulating lipid metabolism in the Long-Evans Cinnamon rat model of Wilson’s disease[J]. Life Sci, 2007, 80( 16): 1472- 1483. DOI: 10.1016/j.lfs.2007.01.017. [7] SEESSLE J, GOHDES A, GOTTHARDT DN, et al. Alterations of lipid metabolism in Wilson disease[J]. Lipids Health Dis, 2011, 10: 83. DOI: 10.1186/1476-511X-10-83. [8] SINTUSEK P, DHAWAN A. Lipid and copper metabolism in humans with Wilson disease: Enigmatic relationship[J]. Hepatology, 2017, 65( 2): 753- 755. DOI: 10.1002/hep.28936. [9] BIERŁA JB, JAŃCZYK W, KONOPKA E, et al. Fatty acid-binding protein 1 as a potential new serological marker of liver status in children with Wilson disease[J]. J Pediatr Gastroenterol Nutr, 2021, 73( 4): 455- 462. DOI: 10.1097/MPG.0000000000003128. [10] ZHI YX, SUN YJ, JIAO YG, et al. HR-MS based untargeted lipidomics reveals characteristic lipid signatures of Wilson’s disease[J]. Front Pharmacol, 2021, 12: 754185. DOI: 10.3389/fphar.2021.754185. [11] CHEN H, WANG X, ZHANG J, et al. Exploration of TCM syndrome types of the material basis and risk prediction of Wilson disease liver fibrosis based on 1H NMR metabolomics[J]. J Pharm Biomed Anal, 2024, 245: 116167. DOI: 10.1016/j.jpba.2024.116167. [12] LIU Q, WU XY, LIU CC, et al. Metabolomic and biochemical changes in the plasma and liver of toxic milk mice model of Wilson disease[J]. J Pharm Biomed Anal, 2024, 246: 116255. DOI: 10.1016/j.jpba.2024.116255. [13] HUSTER D, LUTSENKO S. Wilson disease: Not just a copper disorder. Analysis of a Wilson disease model demonstrates the link between copper and lipid metabolism[J]. Mol Biosyst, 2007, 3( 12): 816- 824. DOI: 10.1039/b711118p. [14] WANG MH, YANG F, ZHANG XZ, et al. Comparative analysis of MTF-1 binding sites between human and mouse[J]. Mamm Genome, 2010, 21( 5-6): 287- 298. DOI: 10.1007/s00335-010-9257-7. [15] HORN CL, MORALES AL, SAVARD C, et al. Role of cholesterol-associated steatohepatitis in the development of NASH[J]. Hepatol Commun, 2022, 6( 1): 12- 35. DOI: 10.1002/hep4.1801. [16] GOTTLIEB A, DEV S, DEVINE L, et al. Hepatic steatosis in the mouse model of Wilson disease coincides with a muted inflammatory response[J]. Am J Pathol, 2022, 192( 1): 146- 159. DOI: 10.1016/j.ajpath.2021.09.010. [17] LIGGI M, MURGIA D, CIVOLANI A, et al. The relationship between copper and steatosis in Wilson’s disease[J]. Clin Res Hepatol Gastroenterol, 2013, 37( 1): 36- 40. DOI: 10.1016/j.clinre.2012.03.038. [18] WANG ZX, XU QY, WANG MY, et al. Metabolic dysfunction-associated steatotic liver disease in patients and mice with Wilson disease[J]. Am J Pathol, 2025, 195( 9): 1600- 1618. DOI: 10.1016/j.ajpath.2025.05.009. [19] STÄTTERMAYER AF, TRAUSSNIGG S, DIENES HP, et al. Hepatic steatosis in Wilson disease: Role of copper and PNPLA3 mutations[J]. J Hepatol, 2015, 63( 1): 156- 163. DOI: 10.1016/j.jhep.2015.01.034. [20] WANG MX, WANG F, TAO Z, et al. Analysis of factors affecting early hepatic steatosis in pediatric patients with Wilson’s disease in China: A retrospective study[J]. Medicine, 2025, 104( 45): e45501. DOI: 10.1097/MD.0000000000045501. [21] MUCHENDITSI A, YANG HJ, HAMILTON JP, et al. Targeted inactivation of copper transporter Atp7b in hepatocytes causes liver steatosis and obesity in mice[J]. Am J Physiol Gastrointest Liver Physiol, 2017, 313( 1): G39- G49. DOI: 10.1152/ajpgi.00312.2016. [22] STÄTTERMAYER AF, TRAUSSNIGG S, AIGNER E, et al. Low hepatic copper content and PNPLA3 polymorphism in non-alcoholic fatty liver disease in patients without metabolic syndrome[J]. J Trace Elem Med Biol, 2017, 39: 100- 107. DOI: 10.1016/j.jtemb.2016.08.006. [23] GAO DJ, ZENG T, CHONG YT, et al. Copper and hepatic lipid dysregulation: Mechanisms and implications[J]. World J Hepatol, 2025, 17( 8): 107803. DOI: 10.4254/wjh.v17.i8.107803. [24] ROBERTS EA, ROBINSON BH, YANG SY. Mitochondrial structure and function in the untreated Jackson toxic milk(tx-j) mouse, a model for Wilson disease[J]. Mol Genet Metab, 2008, 93( 1): 54- 65. DOI: 10.1016/j.ymgme.2007.08.127. [25] OE S, MIYAGAWA K, HONMA Y, et al. Copper induces hepatocyte injury due to the endoplasmic reticulum stress in cultured cells and patients with Wilson disease[J]. Exp Cell Res, 2016, 347( 1): 192- 200. DOI: 10.1016/j.yexcr.2016.08.003. [26] SONG YF, XU YH, ZHUO MQ, et al. CREB element is essential for unfolded protein response(UPR) mediating the Cu-induced changes of hepatic lipogenic metabolism in Chinese yellow catfish(Pelteobagrus fulvidraco)[J]. Aquat Toxicol, 2018, 203: 69- 79. DOI: 10.1016/j.aquatox.2018.08.002. [27] SONG YF, LUO Z, ZHANG LH, et al. Endoplasmic reticulum stress and disturbed calcium homeostasis are involved in copper-induced alteration in hepatic lipid metabolism in yellow catfish Pelteobagrus fulvidraco[J]. Chemosphere, 2016, 144: 2443- 2453. DOI: 10.1016/j.chemosphere.2015.11.031. [28] WOOTON-KEE CR, JAIN AK, WAGNER M, et al. Elevated copper impairs hepatic nuclear receptor function in Wilson’s disease[J]. J Clin Invest, 2015, 125( 9): 3449- 3460. DOI: 10.1172/JCI78991. [29] HAMILTON JP, KOGANTI L, MUCHENDITSI A, et al. Activation of liver X receptor/retinoid X receptor pathway ameliorates liver disease in Atp7b(-/-)(Wilson disease) mice[J]. Hepatology, 2016, 63( 6): 1828- 1841. DOI: 10.1002/hep.28406. [30] SHI YJ, ZOU YX, SHEN ZY, et al. Trace elements, PPARs, and metabolic syndrome[J]. Int J Mol Sci, 2020, 21( 7): 2612. DOI: 10.3390/ijms21072612. [31] NAGASAKA H, MIIDA T, INUI A, et al. Fatty liver and anti-oxidant enzyme activities along with peroxisome proliferator-activated receptors γ and α expressions in the liver of Wilson’s disease[J]. Mol Genet Metab, 2012, 107( 3): 542- 547. DOI: 10.1016/j.ymgme.2012.08.004. [32] WOOTON-KEE CR, ROBERTSON M, ZHOU Y, et al. Metabolic dysregulation in the Atp7b-/- Wilson’s disease mouse model[J]. Proc Natl Acad Sci U S A, 2020, 117( 4): 2076- 2083. DOI: 10.1073/pnas.1914267117. [33] XIE LP, YUAN YM, XU SM, et al. Downregulation of hepatic ceruloplasmin ameliorates NAFLD via SCO1-AMPK-LKB1 complex[J]. Cell Rep, 2022, 41( 3): 111498. DOI: 10.1016/j.celrep.2022.111498. [34] LIU L, FU JP, TANG QY, et al. Combined transcriptomics and metabolomics analysis reveals lipid metabolic disruption in swamp eel(Monopterus albus) under chronic waterborne copper exposure[J]. Aquat Toxicol, 2023, 259: 106520. DOI: 10.1016/j.aquatox.2023.106520. [35] POLISHCHUK EV, MEROLLA A, LICHTMANNEGGER J, et al. Activation of autophagy, observed in liver tissues from patients with Wilson disease and from ATP7B-deficient animals, protects hepatocytes from copper-induced apoptosis[J]. Gastroenterology, 2019, 156( 4): 1173- 1189. DOI: 10.1053/j.gastro.2018.11.032. [36] MELTON PE, BURTON MA, LILLYCROP KA, et al. Differential DNA methylation of steatosis and non-alcoholic fatty liver disease in adolescence[J]. Hepatol Int, 2023, 17( 3): 584- 594. DOI: 10.1007/s12072-022-10469-7. [37] MA JT, NANO J, DING JZ, et al. A peripheral blood DNA methylation signature of hepatic fat reveals a potential causal pathway for nonalcoholic fatty liver disease[J]. Diabetes, 2019, 68( 5): 1073- 1083. DOI: 10.2337/DB18-1193. [38] MEDICI V, SHIBATA NM, KHARBANDA KK, et al. Wilson’s disease: Changes in methionine metabolism and inflammation affect global DNA methylation in early liver disease[J]. Hepatology, 2013, 57( 2): 555- 565. DOI: 10.1002/hep.26047. [39] MORDAUNT CE, KIEFFER DA, SHIBATA NM, et al. Epigenomic signatures in liver and blood of Wilson disease patients include hypermethylation of liver-specific enhancers[J]. Epigenetics Chromatin, 2019, 12( 1): 10. DOI: 10.1186/s13072-019-0255-z. [40] MAZI TA, SHIBATA NM, MEDICI V. Lipid and energy metabolism in Wilson disease[J]. Liver Res, 2020, 4( 1): 5- 14. DOI: 10.1016/j.livres.2020.02.002. [41] FONTES A, PIERSON H, BIERŁA JB, et al. Copper impairs the intestinal barrier integrity in Wilson disease[J]. Metabolism, 2024, 158: 155973. DOI: 10.1016/j.metabol.2024.155973. [42] GUTTMANN S, NADZEMOVA O, GRÜNEWALD I, et al. ATP7B knockout disturbs copper and lipid metabolism in Caco-2 cells[J]. PLoS One, 2020, 15( 3): e0230025. DOI: 10.1371/journal.pone.0230025. [43] MI XX, LI ZH, YAN J, et al. Activation of HIF-1 signaling ameliorates liver steatosis in zebrafish atp7b deficiency(Wilson’s disease) models[J]. Biochim Biophys Acta Mol Basis Dis, 2020, 1866( 10): 165842. DOI: 10.1016/j.bbadis.2020.165842. [44] CHENG CL, WANG Q, HUANG YR, et al. Gandouling inhibits hepatic fibrosis in Wilson’s disease through Wnt-1/β-catenin signaling pathway[J]. J Ethnopharmacol, 2023, 311: 116445. DOI: 10.1016/j.jep.2023.116445. [45] MAZI TA, SARODE GV, CZLONKOWSKA A, et al. Dysregulated choline, methionine, and aromatic amino acid metabolism in patients with Wilson disease: Exploratory metabolomic profiling and implications for hepatic and neurologic phenotypes[J]. Int J Mol Sci, 2019, 20( 23): 5937. DOI: 10.3390/ijms20235937. [46] LI JY, JIANG YL, XU T, et al. Wilson disease with novel compound heterozygote mutations in the ATP7B gene presenting with severe diabetes[J]. Diabetes Care, 2020, 43( 6): 1363- 1365. DOI: 10.2337/dc19-2033. [47] TANG S, LIANG C, YU HT, et al. The potential serum sphingolipid biomarkers for distinguishing Wilson disease[J]. Clin Chim Acta, 2024, 553: 117740. DOI: 10.1016/j.cca.2023.117740. [48] QIU YJ, SU MC, XIAO XN, et al. Metabolomic profiling of Wilson disease, an inherited disorder of copper metabolism, and diseases with similar symptoms but normal copper metabolism[J]. Orphanet J Rare Dis, 2023, 18( 1): 282. DOI: 10.1186/s13023-023-02900-5. [49] DU CY, FUJII Y, ITO M, et al. Dietary polyunsaturated fatty acids suppress acute hepatitis, alter gene expression and prolong survival of female Long-Evans Cinnamon rats, a model of Wilson disease[J]. J Nutr Biochem, 2004, 15( 5): 273- 280. DOI: 10.1016/j.jnutbio.2003.11.005. [50] EINER C, LEITZINGER C, LICHTMANNEGGER J, et al. A high-calorie diet aggravates mitochondrial dysfunction and triggers severe liver damage in Wilson disease rats[J]. Cell Mol Gastroenterol Hepatol, 2019, 7( 3): 571- 596. DOI: 10.1016/j.jcmgh.2018.12.005. [51] MAZI TA, SHIBATA NM, SARODE GV, et al. Hepatic oxylipin profiles in mouse models of Wilson disease: New insights into early hepatic manifestations[J]. Biochim Biophys Acta Mol Cell Biol Lipids, 2024, 1869( 2): 159446. DOI: 10.1016/j.bbalip.2023.159446. [52] MEDICI V, SHIBATA NM, KHARBANDA KK, et al. Maternal choline modifies fetal liver copper, gene expression, DNA methylation, and neonatal growth in the tx-j mouse model of Wilson disease[J]. Epigenetics, 2014, 9( 2): 286- 296. DOI: 10.4161/epi.27110. -



 PDF下载 ( 814 KB)
PDF下载 ( 814 KB)

 下载:
下载:


