原发性胆汁性胆管炎患者疲劳的发生机制及临床评估与干预
DOI: 10.12449/JCH260326
利益冲突声明:本文不存在任何利益冲突。
作者贡献声明:任威瑞负责拟定写作思路,撰写论文;张创、赵文娟负责文献检索,整理内容;王军民负责指导撰写文章并最后定稿。
Pathogenesis, clinical assessment, and intervention of fatigue in patients with primary biliary cholangitis
-
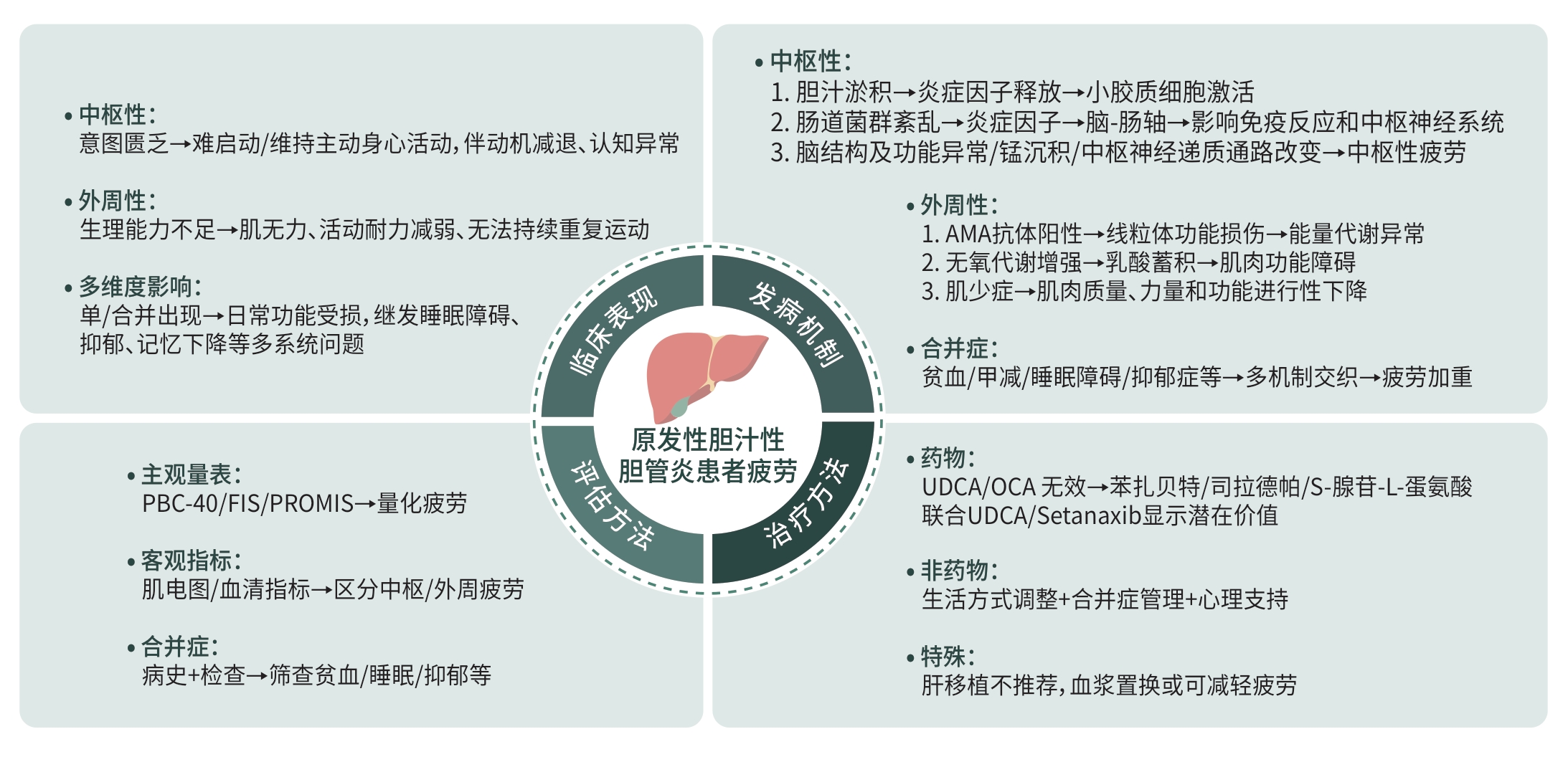
摘要: 原发性胆汁性胆管炎(PBC)是一种以肝内胆汁淤积为特征的自身免疫性肝病,疲劳是其常见且显著影响生活质量的重要症状。PBC患者疲劳的发生机制复杂,可能与胆汁淤积引发的炎症反应、肠道菌群紊乱、脑结构和功能异常以及线粒体功能障碍等因素有关。当前,一线药物和肝移植对改善疲劳的效果有限,且缺乏统一的综合评估体系。新兴药物和生活方式调整等非药物干预手段,则表现出潜在的应用前景。本文系统综述了PBC患者疲劳的临床表现、发生机制、临床评估及干预措施的研究进展,旨在为优化治疗策略和推动新疗法研发提供参考。Abstract: Primary biliary cholangitis (PBC) is an autoimmune liver disease characterized by intrahepatic cholestasis, while fatigue is a common symptom of PBC that significantly affects the quality of life of patients. The pathogenesis of fatigue is complex and may be associated with the factors such as cholestasis-induced inflammation, gut microbiota dysbiosis, brain structural and functional abnormalities, and mitochondrial dysfunction. At present, first-line therapies and liver transplantation have a limited effect in alleviating fatigue, and there is still a lack of standardized comprehensive assessment system. Emerging drugs and non-pharmaceutical interventions, including lifestyle modifications, have shown potential application prospects. This article systematically reviews the research advances in the clinical manifestations, pathogenesis, clinical assessment, and intervention of fatigue in PBC patients, in order to provide a reference for optimizing treatment strategies and promoting the research and development of new therapies.
-
Key words:
- Primary Biliary Cholangitis /
- Fatigue /
- Therapeutics
-
[1] Chinese Society of Hepatology, Chinese Medical Association. Guidelines on the diagnosis and management of primary biliary cholangitis(2021)[J]. J Clin Hepatol, 2022, 38( 1): 35- 41. DOI: 10.3969/j.issn.1001-5256.2022.01.007.中华医学会肝病学分会. 原发性胆汁性胆管炎的诊断和治疗指南(2021)[J]. 临床肝胆病杂志, 2022, 38( 1): 35- 41. DOI: 10.3969/j.issn.1001-5256.2022.01.007. [2] FAISAL A. Understanding fatigue and pruritus in primary biliary cholangitis[J]. Clin Liver Dis, 2024, 23( 1): e0216. DOI: 10.1097/CLD.0000000000000216. [3] LYNCH EN, CAMPANI C, INNOCENTI T, et al. Understanding fatigue in primary biliary cholangitis: From pathophysiology to treatment perspectives[J]. World J Hepatol, 2022, 14( 6): 1111- 1119. DOI: 10.4254/wjh.v14.i6.1111. [4] DYSON JK, WILKINSON N, JOPSON L, et al. The inter-relationship of symptom severity and quality of life in 2055 patients with primary biliary cholangitis[J]. Aliment Pharmacol Ther, 2016, 44( 10): 1039- 1050. DOI: 10.1111/apt.13794. [5] MACHADO MO, KANG NC, TAI F, et al. Measuring fatigue: A meta-review[J]. Int J Dermatol, 2021, 60( 9): 1053- 1069. DOI: 10.1111/ijd.15341. [6] GERBER LH, WEINSTEIN AA, MEHTA R, et al. Importance of fatigue and its measurement in chronic liver disease[J]. World J Gastroenterol, 2019, 25( 28): 3669- 3683. DOI: 10.3748/wjg.v25.i28.3669. [7] KHANNA A, HEGADE VS, JONES DE. Management of fatigue in primary biliary cholangitis[J]. Curr Hepatol Rep, 2019, 18( 2): 127- 133. DOI: 10.1007/s11901-019-00458-0. [8] PHAW NA, DYSON JK, MELLS G, et al. Understanding fatigue in primary biliary cholangitis[J]. Dig Dis Sci, 2021, 66( 7): 2380- 2386. DOI: 10.1007/s10620-020-06502-0. [9] DANTZER R, HEIJNEN CJ, KAVELAARS A, et al. The neuroimmune basis of fatigue[J]. Trends Neurosci, 2014, 37( 1): 39- 46. DOI: 10.1016/j.tins.2013.10.003. [10] JOPSON L, JONES DEJ. Fatigue in primary biliary cirrhosis: Prevalence, pathogenesis and management[J]. Dig Dis, 2015, 33( Suppl 2): 109- 114. DOI: 10.1159/000440757. [11] D'MELLO C, LE T, SWAIN MG. Cerebral microglia recruit monocytes into the brain in response to tumor necrosis factoralpha signaling during peripheral organ inflammation[J]. J Neurosci, 2009, 29( 7): 2089- 2102. DOI: 10.1523/JNEUROSCI.3567-08.2009. [12] TOUSSAINT A, BUCK L, HARTL J, et al. Factors associated with severity and persistence of fatigue in patients with primary biliary cholangitis: Study protocol of a prospective cohort study with a mixed-methods approach(SOMA.LIV)[J]. BMJ Open, 2022, 12( 12): e061419. DOI: 10.1136/bmjopen-2022-061419. [13] MOSHER VAL, SWAIN MG, PANG JXQ, et al. Primary biliary cholangitis alters functional connections of the brain's deep gray matter[J]. Clin Transl Gastroenterol, 2017, 8( 7): e107. DOI: 10.1038/ctg.2017.34. [14] NEWTON JL, HOLLINGSWORTH KG, TAYLOR R, et al. Cognitive impairment in primary biliary cirrhosis: Symptom impact and potential etiology[J]. Hepatology, 2008, 48( 2): 541- 549. DOI: 10.1002/hep.22371. [15] MCDONALD C, NEWTON J, LAI HM, et al. Central nervous system dysfunction in primary biliary cirrhosis and its relationship to symptoms[J]. J Hepatol, 2010, 53( 6): 1095- 1100. DOI: 10.1016/j.jhep.2010.05.036. [16] ZHAO J, CAO J, YAO DK. Research advances in pathogenesis and management of fatigue in patients with primary biliary cirrhosis[J]. J Clin Hepatol, 2016, 32( 11): 2218- 2221. DOI: 10.3969/j.issn.1001-5256.2016.11.050.赵健, 曹嘉, 姚定康. 原发性胆汁性胆管炎乏力机制与治疗进展[J]. 临床肝胆病杂志, 2016, 32( 11): 2218- 2221. DOI: 10.3969/j.issn.1001-5256.2016.11.050. [17] FORTON DM, PATEL N, PRINCE M, et al. Fatigue and primary biliary cirrhosis: Association of globus pallidus magnetisation transfer ratio measurements with fatigue severity and blood manganese levels[J]. Gut, 2004, 53( 4): 587- 592. DOI: 10.1136/gut.2003.016766. [18] TALWALKAR JA, DONLINGER JJ, GOSSARD AA, et al. Fluoxetine for the treatment of fatigue in primary biliary cirrhosis: A randomized, double-blind controlled trial[J]. Dig Dis Sci, 2006, 51( 11): 1985- 1991. DOI: 10.1007/s10620-006-9397-5. [19] THEAL JJ, TOOSI MN, GIRLAN L, et al. A randomized, controlled crossover trial of ondansetron in patients with primary biliary cirrhosis and fatigue[J]. Hepatology, 2005, 41( 6): 1305- 1312. DOI: 10.1002/hep.20698. [20] LI MJ, SUN JG. Research progress on fatigue mechanism of primary biliary cholangitis[J]. Chin J Integr Tradit West Med Liver Dis, 2020, 30( 6): 574- 576. DOI: 10.3969/j.issn.1005-0264.2020.06.002.李明津, 孙建光. 原发性胆汁性胆管炎疲劳机制研究进展[J]. 中西医结合肝病杂志, 2020, 30( 6): 574- 576. DOI: 10.3969/j.issn.1005-0264.2020.06.002. [21] HOLLINGSWORTH KG, NEWTON JL, TAYLOR R, et al. Pilot study of peripheral muscle function in primary biliary cirrhosis: Potential implications for fatigue pathogenesis[J]. Clin Gastroenterol Hepatol, 2008, 6( 9): 1041- 1048. DOI: 10.1016/j.cgh.2008.04.013. [22] YANG JQ, JIANG SS, FAN QL, et al. Prevalence and effect on prognosis of sarcopenia in patients with primary biliary cholangitis[J]. Front Med, 2024, 11: 1346165. DOI: 10.3389/fmed.2024.1346165. [23] SAEKI C, OIKAWA T, KANAI T, et al. Relationship between osteoporosis, sarcopenia, vertebral fracture, and osteosarcopenia in patients with primary biliary cholangitis[J]. Eur J Gastroenterol Hepatol, 2021, 33( 5): 731- 737. DOI: 10.1097/MEG.0000000000001791. [24] ZHANG JT, KONG M, GENG N, et al. Progress in the treatment of sarcopenia in patients with cirrhosis[J]. Chin J Hepatol, 2023, 31( 12): 1340- 1344. DOI: 10.3760/cma.j.cn501113-20231126-00237.张家腾, 孔明, 耿楠, 等. 肝硬化患者肌肉减少症的治疗进展[J]. 中华肝脏病杂志, 2023, 31( 12): 1340- 1344. DOI: 10.3760/cma.j.cn501113-20231126-00237. [25] BAUTMANS I, GORUS E, NJEMINI R, et al. Handgrip performance in relation to self-perceived fatigue, physical functioning and circulating IL-6 in elderly persons without inflammation[J]. BMC Geriatr, 2007, 7: 5. DOI: 10.1186/1471-2318-7-5. [26] CHEN M, MA N, JIN JB, et al. A case of primary biliary cholangitis with megaloblastic anemia[J]. J Clin Hepatol, 2022, 38( 5): 1114- 1115. DOI: 10.3969/j.issn.1001-5256.2022.05.026.陈梅, 马宁, 金敬波, 等. 原发性胆汁性胆管炎合并巨幼细胞性贫血1例报告[J]. 临床肝胆病杂志, 2022, 38( 5): 1114- 1115. DOI: 10.3969/j.issn.1001-5256.2022.05.026. [27] ZHANG XX, FENG LN, CHEN QL, et al. Anemia caused by primary biliary cholangitis and special reasons: A case report[J]. J Clin Hepatol, 2020, 36( 4): 885- 887. DOI: 10.3969/j.issn.1001-5256.2020.04.038.张晓雪, 冯丽娜, 陈庆灵, 等. 原发性胆汁性胆管炎合并特殊原因所致贫血1例报告[J]. 临床肝胆病杂志, 2020, 36( 4): 885- 887. DOI: 10.3969/j.issn.1001-5256.2020.04.038. [28] WU R, LENG AM. Primary biliary cirrhosis with autoimmune hemolytic anemia: A case report[J]. J Clin Hepatol, 2020, 36( 12): 2795- 2797. DOI: 10.3969/j.issn.1001-5256.2020.12.030.吴蓉, 冷爱民. 原发性胆汁性胆管炎合并自身免疫性溶血性贫血1例报告[J]. 临床肝胆病杂志, 2020, 36( 12): 2795- 2797. DOI: 10.3969/j.issn.1001-5256.2020.12.030. [29] HOU YQ. Association study between the occurrence and development of primary biliary cholangitis and thyroid function[D]. Nanjing: Nanjing Medical University, 2022. DOI: 10.27249/d.cnki.gnjyu.2022.000184.侯雨晴. 原发性胆汁性胆管炎的发生发展与甲状腺功能的关联研究[D]. 南京: 南京医科大学, 2022. DOI: 10.27249/d.cnki.gnjyu.2022.000184. [30] YAN YT, JIA G, MENG Q, et al. Thyroid functions and their impact on response to standardized therapy in patients with autoimmune hepatitis and primary biliary cholangitis[J]. J Pract Hepatol, 2024, 27( 1): 52- 55. DOI: 10.3969/j.issn.1672-5069.2024.01.014.闫玉婷, 贾桂, 孟琴, 等. 自身免疫性肝炎和原发性胆汁性胆管炎患者甲状腺功能变化及其对治疗应答的影响[J]. 实用肝脏病杂志, 2024, 27( 1): 52- 55. DOI: 10.3969/j.issn.1672-5069.2024.01.014. [31] ZHAO CY. Sleep disorders, mental health and related factors in patients with primary biliary cholangitis[D]. Qingdao: Qingdao University, 2023. DOI: 10.27262/d.cnki.gqdau.2023.000422.赵晨阳. 原发性胆汁性胆管炎患者睡眠障碍、心理健康及相关因素研究[D]. 青岛: 青岛大学, 2023. DOI: 10.27262/d.cnki.gqdau.2023.000422. [32] ZISAPEL N. Sleep and sleep disturbances: Biological basis and clinical implications[J]. Cell Mol Life Sci, 2007, 64( 10): 1174. DOI: 10.1007/s00018-007-6529-9. [33] STONE EA, LIN Y, QUARTERMAIN D. A final common pathway for depression? Progress toward a general conceptual framework[J]. Neurosci Biobehav Rev, 2008, 32( 3): 508- 524. DOI: 10.1016/j.neubiorev.2007.08.007. [34] YIRMIYA R. The inflammatory underpinning of depression: An historical perspective[J]. Brain Behav Immun, 2024, 122: 433- 443. DOI: 10.1016/j.bbi.2024.08.048. [35] SIVAKUMAR T, KOWDLEY KV. Anxiety and depression in patients with primary biliary cholangitis: Current insights and impact on quality of life[J]. Hepat Med, 2021, 13: 83- 92. DOI: 10.2147/HMER.S256692. [36] JACOBY A, RANNARD A, BUCK D, et al. Development, validation, and evaluation of the PBC-40, a disease specific health related quality of life measure for primary biliary cirrhosis[J]. Gut, 2005, 54( 11): 1622- 1629. DOI: 10.1136/gut.2005.065862. [37] FISK JD, RITVO PG, ROSS L, et al. Measuring the functional impact of fatigue: Initial validation of the fatigue impact scale[J]. Clin Infect Dis, 1994, 18( Suppl 1): S79- S83. DOI: 10.1093/clinids/18.supplement_1.s79. [38] CELLA D, RILEY W, STONE A, et al. The Patient-Reported Outcomes Measurement Information System(PROMIS) developed and tested its first wave of adult self-reported health outcome item banks: 2005-2008[J]. J Clin Epidemiol, 2010, 63( 11): 1179- 1194. DOI: 10.1016/j.jclinepi.2010.04.011. [39] FINSTERER J. Biomarkers of peripheral muscle fatigue during exercise[J]. BMC Musculoskelet Disord, 2012, 13: 218. DOI: 10.1186/1471-2474-13-218. [40] CIFREK M, MEDVED V, TONKOVIĆ S, et al. Surface EMG based muscle fatigue evaluation in biomechanics[J]. Clin Biomech, 2009, 24( 4): 327- 340. DOI: 10.1016/j.clinbiomech.2009.01.010. [41] LAURENT A, PLAMONDON R, BEGON M. Central and peripheral shoulder fatigue pre-screening using the sigma-lognormal model: A proof of concept[J]. Front Hum Neurosci, 2020, 14: 171. DOI: 10.3389/fnhum.2020.00171. [42] GANDEVIA SC. Spinal and supraspinal factors in human muscle fatigue[J]. Physiol Rev, 2001, 81( 4): 1725- 1789. DOI: 10.1152/physrev.2001.81.4.1725. [43] NEWTON JL, GIBSON GJ, TOMLINSON M, et al. Fatigue in primary biliary cirrhosis is associated with excessive daytime somnolence[J]. Hepatology, 2006, 44( 1): 91- 98. DOI: 10.1002/hep.21230. [44] VAN OS E, VAN DEN BROEK WW, MULDER PGH, et al. Depression in patients with primary biliary cirrhosis and primary sclerosing cholangitis[J]. J Hepatol, 2007, 46( 6): 1099- 1103. DOI: 10.1016/j.jhep.2007.01.036. [45] HARMS MH, VAN BUUREN HR, CORPECHOT C, et al. Ursodeoxycholic acid therapy and liver transplant-free survival in patients with primary biliary cholangitis[J]. J Hepatol, 2019, 71( 2): 357- 365. DOI: 10.1016/j.jhep.2019.04.001. [46] ANGULO P, DICKSON ER, THERNEAU TM, et al. Comparison of three doses of ursodeoxycholic acid in the treatment of primary biliary cirrhosis: A randomized trial[J]. J Hepatol, 1999, 30( 5): 830- 835. DOI: 10.1016/s0168-8278(99)80136-6. [47] HIRSCHFIELD GM, MASON A, LUKETIC V, et al. Efficacy of obeticholic acid in patients with primary biliary cirrhosis and inadequate response to ursodeoxycholic acid[J]. Gastroenterology, 2015, 148( 4): 751- 761. DOI: 10.1053/j.gastro.2014.12.005. [48] CORPECHOT C, CHAZOUILLÈRES O, ROUSSEAU A, et al. A placebo-controlled trial of bezafibrate in primary biliary cholangitis[J]. N Engl J Med, 2018, 378( 23): 2171- 2181. DOI: 10.1056/NEJMoa1714519. [49] HIRSCHFIELD GM, BOWLUS CL, MAYO MJ, et al. A phase 3 trial of seladelpar in primary biliary cholangitis[J]. N Engl J Med, 2024, 390( 9): 783- 794. DOI: 10.1056/nejmoa2312100. [50] KREMER AE, MAYO MJ, HIRSCHFIELD G, et al. Seladelpar improved measures of pruritus, sleep, and fatigue and decreased serum bile acids in patients with primary biliary cholangitis[J]. Liver Int, 2022, 42( 1): 112- 123. DOI: 10.1111/liv.15039. [51] WUNSCH E, RASZEJA-WYSZOMIRSKA J, BARBIER O, et al. Effect of S-adenosyl-L-methionine on liver biochemistry and quality of life in patients with primary biliary cholangitis treated with ursodeoxycholic acid. A prospective, open label pilot study[J]. J Gastrointestin Liver Dis, 2018, 27( 3): 273- 279. DOI: 10.15403/jgld.2014.1121.273.icz. [52] VÖGELIN M, KREMER AE. Advancing care in primary biliary cholangitis: Emerging insights and novel therapies[J]. Expert Opin Pharmacother, 2025, 26( 10): 1149- 1162. DOI: 10.1080/14656566.2025.2516622. [53] ZHANG F, LI WJ. Vitamin D and sarcopenia in the senior people: A review of mechanisms and comprehensive prevention and treatment strategies[J]. Ther Clin Risk Manag, 2024, 20: 577- 595. DOI: 10.2147/TCRM.S471191. [54] HIRSCHFIELD GM, DYSON JK, ALEXANDER GJM, et al. The British Society of Gastroenterology/UK-PBC primary biliary cholangitis treatment and management guidelines[J]. Gut, 2018, 67( 9): 1568- 1594. DOI: 10.1136/gutjnl-2017-315259. [55] FREER A, WILLIAMS F, DURMAN S, et al. Home-based exercise in patients with refractory fatigue associated with primary biliary cholangitis: A protocol for the EXerCise Intervention in cholesTatic LivEr Disease(EXCITED) feasibility trial[J]. BMJ Open Gastroenterol, 2021, 8( 1): e000579. DOI: 10.1136/bmjgast-2020-000579. [56] HOLLINGSWORTH KG, NEWTON JL, ROBINSON L, et al. Loss of capacity to recover from acidosis in repeat exercise is strongly associated with fatigue in primary biliary cirrhosis[J]. J Hepatol, 2010, 53( 1): 155- 161. DOI: 10.1016/j.jhep.2010.02.022. [57] TURCO M, CAZZAGON N, FRANCESCHET I, et al. Morning bright light treatment for sleep-wake disturbances in primary biliary cholangitis: A pilot study[J]. Front Physiol, 2018, 9: 1530. DOI: 10.3389/fphys.2018.01530. [58] ZHENG YJ, JI PZ, FENG P, et al. Research progress in traditional Chinese medicine treatment of chronic fatigue syndrome with yang deficiency of spleen and kidney[J]. J Changchun Univ Chin Med, 2024, 40( 10): 1156- 1161. DOI: 10.13463/j.cnki.cczyy.2024.10.021.张渝婧, 仉培臻, 奉飘, 等. 脾肾阳虚型慢性疲劳综合征的中医治疗研究进展[J]. 长春中医药大学学报, 2024, 40( 10): 1156- 1161. DOI: 10.13463/j.cnki.cczyy.2024.10.021. [59] European Association for the Study of the Liver. EASL Clinical Practice Guidelines: The diagnosis and management of patients with primary biliary cholangitis[J]. J Hepatol, 2017, 67( 1): 145- 172. DOI: 10.1016/j.jhep.2017.03.022. [60] WUNSCH E, KRUK B, SNARSKI E, et al. Plasmapheresis in the treatment of chronic fatigue in patients with primary biliary cholangitis[J]. Pol Arch Intern Med, 2021, 131( 2): 205- 207. DOI: 10.20452/pamw.15690. -



 PDF下载 ( 778 KB)
PDF下载 ( 778 KB)

 下载:
下载:


