ALBI评分对肝硬化食管胃底静脉曲张破裂出血患者预后的预测价值
DOI: 10.3969/j.issn.1001-5256.2021.03.017
利益冲突声明:本研究不存在研究者、伦理委员会成员、受试者监护人以及与公开研究成果有关的利益冲突,特此声明。
作者贡献声明:孙梦园负责收集数据,课题设计,资料分析,撰写论文;向晓星负责拟定写作思路,指导撰写文章,修改论文并最后定稿。
Value of albumin-bilirubin score in predicting the prognosis of cirrhotic patients with esophagogastric variceal bleeding
-
摘要:
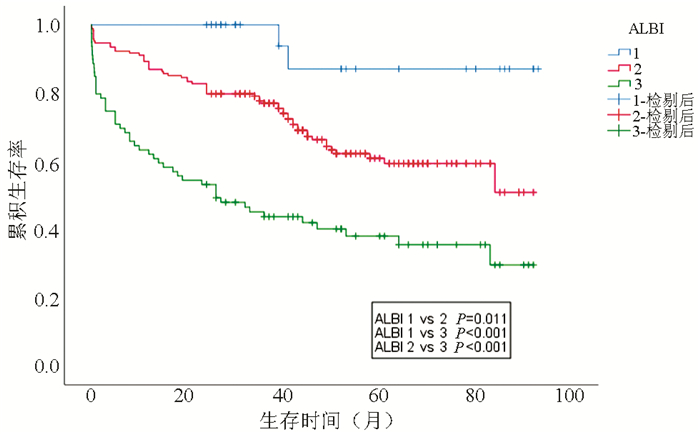
目的 研究ALBI评分预测肝硬化伴食管胃底静脉曲张破裂出血患者预后的价值,以明确风险分层和增加临床实用性。 方法 回顾性分析2012年10月—2018年8月于江苏省苏北人民医院住院治疗的273例肝硬化食管胃底静脉曲张破裂出血患者的临床资料,所有患者入院后均接受标准化治疗,通过查阅电子病历及电话随访获取患者的生存情况,根据随访至2020年8月时的预后情况分为死亡组(n=109)和存活组(n=164),比较两组患者的一般资料,连续变量两组间比较采用Mann-Whitney U检验,分类变量两组间比较采用χ2检验或Fisher确切检验,通过单因素及多因素Cox回归分析识别与预后相关的独立危险因素,运用Kaplan-Meier曲线分析不同ALBI分级患者的生存率,并行log-rank检验进行组间比较,绘制受试者工作特征曲线(ROC曲线)比较ALBI评分、CTP评分及MELD评分预测患者短期(6周)及长期预后的能力。 结果 随访期间,109例(39.9%)患者死亡,死亡组患者的ALBI评分[-1.49(-1.82~-1.11)]水平明显高于存活组[-1.79(-2.22~-1.49)](Z=5.630, P<0.001)。单因素分析显示:年龄≥55岁、血红蛋白≤100 g/L、中性粒细胞计数≥3.4×109/L、血小板≤42×109/L、白蛋白≤28 g/L、总胆红素≥21 μmol/L、ALT≥42 U/L或AST≥48 U/L、肌酐≥94 μmol/L、血钠≤137 mmol/L、凝血酶原标准化比值≥1.5、腹水、肝性脑病为肝硬化EGVB患者死亡的危险因素,且ALBI分级为3级的患者较1级和2级患者的死亡风险明显升高,而预防性套扎为肝硬化食管胃底静脉曲张破裂出血患者生存改善的保护性因素(P值均<0.05)。多因素分析显示:年龄≥55岁[HR(95%CI):2.531(1.624~3.946),P<0.001]、肌酐≥94 μmol /L[HR(95%CI):1.935(1.208~3.100),P=0.006]、血钠≤137 mmol/L[HR(95%CI):1.519(1.015~2.274),P=0.042]、腹水[HR(95%CI):1.641(1.041~2.585),P=0.033]、肝性脑病[HR(95%CI):9.972(3.961~25.106),P<0.001]、ALBI 3级[HR(95%CI):1.591(1.007~2.515),P=0.047]为死亡的独立危险因素。ALBI 3级患者的生存率明显低于ALBI 1级(χ2=18.691, P<0.001)和ALBI 2级(χ2=21.364,P<0.001),ALBI 1级患者的生存率高于ALBI 2级(χ2=6.513,P=0.011)。ROC曲线分析显示在预测短期(6周)及长期预后方面,ALBI评分、CTP评分及MELD评分的ROC曲线下面积分别为0.770、0.730、0.706和0.701、0.685、0.659。 结论 ALBI评分对肝硬化食管胃底静脉曲张破裂出血患者短期(6周)及长期预后具有较好的预测价值,患者的死亡风险随ALBI分级的升高而升高,ALBI评分作为一个客观、简单的模型可更好的应用于临床。 Abstract:Objective To investigate the value of albumin-bilirubin (ALBI) score in predicting the prognosis of cirrhotic patients with esophagogastric variceal bleeding, and to identify risk stratification and increase clinical applicability. Methods A retrospective analysis was performed for the clinical data of 273 cirrhotic patients with esophagogastric variceal bleeding who were hospitalized in Subei People's Hospital of Jiangsu from October 2012 to August 2018, and all patients received standard management after admission. Survival status was obtained through electronic medical records and telephone follow-up, and according to the prognosis in August 2020, the patients were divided into death group with 109 patients and survival group with 164 patients. General data were compared between the two groups. The Mann-Whitney U test was used for comparison of continuous variables between two groups, and the chi-square test or the Fisher's exact test was used for comparison of categorical variables between two groups; univariate and multivariate Cox regression analyses were used to identify independent risk factors for prognosis. The Kaplan-Meier curve was used to analyze the survival rates of patients with different ALBI grades, and the log-rank test was used for comparison between groups; the receiver operating characteristic (ROC) curve was plotted to compare the ability of ALBI score, Child-Turcotte-Pugh (CTP) score, and Model for End-Stage Liver Disease (MELD) score in predicting short-term (6 weeks) and long-term prognoses. Results During follow-up, 109 patients (39.9%) died, and the death group had a significantly higher ALBI score than the survival group [-1.49 (-1.82 to-1.11) vs-1.79 (-2.22 to-1.49), Z=5.630, P < 0.001]. The univariate analysis showed that age ≥55 years, hemoglobin ≤100 g/L, neutrophil count ≥3.4×109/L, platelet count ≤42×109/L, albumin ≤28 g/L, total bilirubin ≥21 μmol/L, alanine aminotransferase ≥42 U/L or aspartate aminotransferase ≥48 U/L, creatinine ≥94 μmol/L, serum sodium ≤137 mmol/L, international normalized ratio of prothrombin ≥1.5, ascites, and hepatic encephalopathy were risk factors for death in cirrhotic patients with esophagogastric variceal bleeding, and the patients with ALBI grade 3 had a significantly higher risk of death than those with ALBI grade 1 or 2; prophylactic ligation was a protective factor for survival improvement in cirrhotic patients with esophagogastric variceal bleeding (all P < 0.05). The multivariate analysis showed that age ≥55 years (hazard ratio [HR]=2.531, 95% confidence interval [CI]: 1.624-3.946, P < 0.001), creatinine ≥94 μmol/L (HR=1.935, 95% CI: 1.208-3.100, P=0.006), serum sodium ≤137 mmol/L [HR=1.519, 95% CI: 1.015-2.274, P=0.042], ascites (HR=1.641, 95% CI: 1.041-2.585, P=0.033), hepatic encephalopathy (HR=9.972, 95% CI: 3.961-25.106, P < 0.001), and ALBI grade 3 (HR=1.591, 95% CI: 1.007-2.515, P=0.047) were independent risk factors for death. The patients with ALBI grade 3 had a significantly lower survival rate than those with ALBI grade 1 (χ2=18.691, P < 0.001) and ALBI grade 2 (χ2=21.364, P < 0.001), and the patients with ALBI grade 1 had a significantly higher survival rate than those with ALBI grade 2 (χ2=6.513, P=0.011). The ROC curve analysis showed that ALBI score, CTP score, and MELD score had an area under the ROC curve (AUC) of 0.770, 0.730, and 0.706, respectively, in predicting short-term (6 weeks) prognosis, and they had an AUC of 0.701, 0.685, and 0.659, respectively, in predicting long-term prognosis. Conclusion ALBI score has a good value in predicting short-term (6 weeks) and long-term prognoses of cirrhotic patients with esophagogastric variceal bleeding, and the risk of death increases with ALBI grade. ALBI score can be used as an objective and simple model in clinical practice. -
Key words:
- Albumin-Bilirubin Score /
- Liver Cirrhosis /
- Esophageal and Gastric Varices /
- Prognosis
-
表 1 存活组与死亡组的临床及生化特征比较
变量 死亡组(n=109) 存活组(n=164) 统计值 P值 男性[例(%)] 67(61.5) 104(63.4) χ2=0.106 0.745 年龄(岁) 62(55~68) 58(48~66) Z=2.894 0.004 病因[例(%)] χ2=0.719 0.869 乙型肝炎 51(46.8) 85(51.8) 丙型肝炎 8(7.3) 12(7.3) 酒精性肝病 6(5.5) 8(4.9) 其他 44(40.4) 59(36.0) 高血压[例(%)] 19(17.4) 36(22.0) χ2=0.832 0.362 糖尿病[例(%)] 22(20.2) 35(21.3) χ2=0.053 0.818 既往EGVB[例(%)] 30(27.5) 35(21.3) χ2=1.379 0.240 实验室指标 血红蛋白(g/L) 82(60~96) 87(65~104) Z=-1.970 0.049 中性粒细胞(×109/L) 4.4(2.7~6.6) 4.0(2.3~6.0) Z=1.473 0.141 淋巴细胞(×109/L) 1.0(0.6~1.4) 0.9(0.6~1.4) Z=0.893 0.372 血小板(×109/L) 69(48~96) 71(52~91) Z=-0.311 0.756 白蛋白(g/L) 29(25~31) 31(28~36) Z=-5.273 <0.001 总胆红素(μmol/L) 23.0(15.0~35.0) 19.3(13.2~28.3) Z=2.266 0.023 ALT(U/L) 37(27~56) 32(23~44) Z=2.352 0.019 AST(U/L) 37(29~63) 35(26~54) Z=1.712 0.087 肌酐(μmol/L) 71(58~92) 71(54~80) Z=1.572 0.116 血钠(mmol/L) 137(134~141) 140(137~142) Z=-3.416 0.001 凝血酶原标准化比值 1.5(1.3~1.7) 1.4(1.3~1.6) Z=3.127 0.002 门静脉血栓[例(%)] 5(4.6) 5(3.0) 0.527 腹水[例(%)] 83(76.1) 94(57.3) χ2=10.183 0.001 肝性脑病[例(%)] 6(5.5) 0 0.004 预防性套扎[例(%)] 8(7.3) 25(15.2) χ2=3.850 0.050 CTP评分 8(7~10) 7(6~8) Z=5.236 <0.001 MELD评分 13(11~15) 11(10~13) Z=4.463 <0.001 ALBI评分 -1.49(-1.82~-1.11) -1.79(-2.22~-1.49) Z=5.630 <0.001 ALBI分级[例(%)] χ2=29.393 <0.001 1 2(1.8) 24(14.6) 2 58(53.2) 110(67.1) 3 49(45.0) 30(18.3) 表 2 肝硬化EGVB患者预后的单因素和多因素分析
变量 单因素分析 多因素分析 HR(95%CI) P值 HR(95%CI) P值 年龄(<55岁 vs ≥55岁) 2.224(1.437~3.442) <0.001 2.531(1.624~3.946) <0.001 既往EGVB(否 vs 是) 1.281(0.841~1.951) 0.249 血红蛋白(>100 g/L vs ≤100 g/L) 1.719(1.058~2.793) 0.029 1.381(0.823~2.319) 0.222 中性粒细胞计数(<3.4×109/L vs ≥3.4×109/L) 1.538(1.029~2.300) 0.036 1.327(0.861~2.045) 0.200 淋巴细胞计数(>0.3×109/L vs ≤0.3 ×109/L) 1.744(0.765~3.975) 0.186 血小板(>42×109/L vs ≤42×109/L) 1.749(1.103~2.773) 0.017 1.447(0.882~2.373) 0.143 白蛋白(>28 g/L vs ≤28 g/L) 2.421(1.660~3.529) <0.001 总胆红素(<21 μmol/L vs ≥21 μmol/L) 1.529(1.044~2.240) 0.029 ALT/AST(ALT<42 U/L,AST<48 U/L vs ALT≥42 U/L,AST≥48 U/L) 1.576(1.081~2.297) 0.018 1.457(0.968~2.192) 0.071 肌酐(<94 μmol/L vs ≥94 μmol/L) 1.933(1.236~3.023) 0.004 1.935(1.208~3.100) 0.006 血钠(>137 mmol/L vs ≤137 mmol/L) 1.975(1.350~2.889) <0.001 1.519(1.015~2.274) 0.042 凝血酶原标准化比值(<1.5 vs ≥1.5) 1.749(1.200~2.548) 0.004 1.307(0.863~1.981) 0.207 门静脉血栓(否 vs 是) 1.553(0.633~3.814) 0.336 腹水(否 vs 是) 1.953(1.256~3.035) 0.003 1.641(1.041~2.585) 0.033 肝性脑病(否 vs 是) 10.265(4.384~24.035) <0.001 9.972(3.961~25.106) <0.001 预防性套扎(否 vs 是) 0.431(0.210~0.887) 0.022 0.527(0.253~1.100) 0.088 ALBI分级(1/2 vs 3) 2.726(1.867~3.981) <0.001 1.591(1.007~2.515) 0.047 -
[1] KOVACS T, JENSEN DM. Varices: Esophageal, gastric, and rectal[J]. Clin Liver Dis, 2019, 23(4): 625-642. DOI: 10.1016/j.cld.2019.07.005 [2] MANDAL AK, PAUDEL MS, KC S, et al. Factors predicting mortality of acute variceal bleeding in liver cirrhosis[J]. JNMA J Nepal Med Assoc, 2018, 56(209): 493-496. DOI: 10.31729/jnma.3408 [3] FORTUNE BE, GARCIA-TSAO G, CIARLEGLIO M, et al. Child-Turcotte-Pugh class is best at stratifying risk in variceal hemorrhage: Analysis of a US multicenter prospective study[J]. J Clin Gastroenterol, 2017, 51(5): 446-453. DOI: 10.1097/MCG.0000000000000733 [4] WANG J, ZHANG Z, YAN X, et al. Albumin-Bilirubin (ALBI) as an accurate and simple prognostic score for chronic hepatitis B-related liver cirrhosis[J]. Dig Liver Dis, 2019, 51(8): 1172-1178. DOI: 10.1016/j.dld.2019.01.011 [5] HSIEH YC, LEE KC, WANG YW, et al. Correlation and prognostic accuracy between noninvasive liver fibrosis markers and portal pressure in cirrhosis: Role of ALBI score[J]. PLoS One, 2018, 13(12): e0208903. DOI: 10.1371/journal.pone.0208903 [6] Chinese Society of Hepatology and Chinese Society of Infectious Diseases, Chinese Medical Association. The guideline of prevention andtreatment for chronic hepatitis B: A 2015 update[J]. J Clin Hepatol, 2015, 31(12): 1941-1960. (in Chinese) DOI: 10.3969/j.issn.1001-5256.2015.12.002中华医学会肝病学分会, 中华医学会感染病学分会. 慢性乙型肝炎防治指南(2015年更新版)[J]. 临床肝胆病杂志, 2015, 31(12): 1941-1960. DOI: 10.3969/j.issn.1001-5256.2015.12.002 [7] XU XY, DING HG, JIA JD, et al. Guidelines for the diagnosis and treatment of esophageal and gastric variceal bleeding in cirrhotic portal hypertension[J]. J Clin Hepatol, 2016, 32(2): 203-219. (in Chinese) DOI: 10.3969/j.issn.1001-5256.2016.02.002徐小元, 丁惠国, 贾继东, 等. 肝硬化门静脉高压食管胃静脉曲张出血的防治指南[J]. 临床肝胆病杂志, 2016, 32(2): 203-219. DOI: 10.3969/j.issn.1001-5256.2016.02.002 [8] JOHNSON PJ, BERHANE S, KAGEBAYASHI C, et al. Assessment of liver function in patients with hepatocellular carcinoma: A new evidence-based approach-the ALBI grade[J]. J Clin Oncol, 2015, 33(6): 550-558. DOI: 10.1200/JCO.2014.57.9151 [9] de FRANCHIS R, Baveno Ⅵ Faculty. Expanding consensus in portal hypertension: Report of the Baveno Ⅵ Consensus Workshop: Stratifying risk and individualizing care for portal hypertension[J]. J Hepatol, 2015, 63(3): 743-752. DOI: 10.1016/j.jhep.2015.05.022 [10] TANTAI XX, LIU N, YANG LB, et al. Prognostic value of risk scoring systems for cirrhotic patients with variceal bleeding[J]. World J Gastroenterol, 2019, 25(45): 6668-6680. DOI: 10.3748/wjg.v25.i45.6668 [11] WU SL, ZHENG YX, TIAN ZW, et al. Scoring systems for prediction of mortality in decompensated liver cirrhosis: A meta-analysis of test accuracy[J]. World J Clin Cases, 2018, 6(15): 995-1006. DOI: 10.12998/wjcc.v6.i15.995 [12] FUJITA K, NOMURA T, MORISHITA A, et al. Prediction of transplant-free survival through albumin-bilirubin score in primary biliary cholangitis[J]. J Clin Med, 2019, 8(8): 1258. DOI: 10.3390/jcm8081258 [13] Chinese Society of Hepatogy, Chinese MedicalAssociation. Chinese guidelines on the management of liver cirrhosis[J]. J Clin Hepatol, 2019, 35(11): 2408-2425. (in Chinese) DOI: 10.3969/j.issn.1001-5256.2019.11.006中华医学会肝病学分会. 肝硬化诊治指南[J]. 临床肝胆病杂志, 2019, 35(11): 2408-2425. DOI: 10.3969/j.issn.1001-5256.2019.11.006 [14] PUENTE A, HERNÁNDEZ-GEA V, GRAUPERA I, et al. Drugs plus ligation to prevent rebleeding in cirrhosis: An updated systematic review[J]. Liver Int, 2014, 34(6): 823-833. DOI: 10.1111/liv.12452 [15] BRUNNER F, BERZIGOTTI A, BOSCH J. Prevention and treatment of variceal haemorrhage in 2017[J]. Liver Int, 2017, 37(Suppl 1): 104-115. http://www.ncbi.nlm.nih.gov/pubmed/28052623 [16] Chinese Society of Spleen and Portal Hypertension Surgery, Chinese Society of Surgery, Chinese Medical Association. Expert consensus on diagnosis and treatment of esophagogastric variceal bleeding in cirrhotic portal hypertension (2019 edition)[J]. Chin J Dig Surg, 2019, 18(12): 1087-1093. (in Chinese)中华医学会外科学分会脾及门静脉高压外科学组. 肝硬化门静脉高压症食管、胃底静脉曲张破裂出血诊治专家共识(2019版)[J]. 中华消化外科杂志, 2019, 18(12): 1087-1093. -



 PDF下载 ( 2118 KB)
PDF下载 ( 2118 KB)

 下载:
下载:



