高原地区内镜微创保胆取石术后结石复发新型预测列线图的构建和验证
DOI: 10.3969/j.issn.1001-5256.2021.03.028
Construction and verification of a new nomogram for predicting stone recurrence after endoscopic minimally invasive gallbladder-preserving cholecystolithotomy at high altitude
-
摘要:
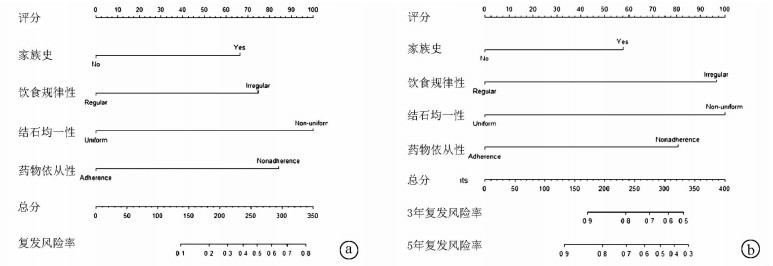
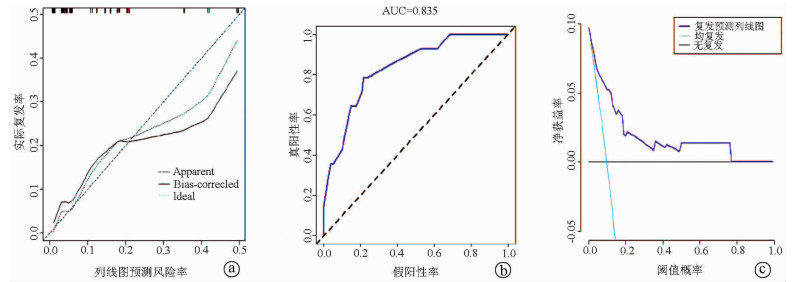
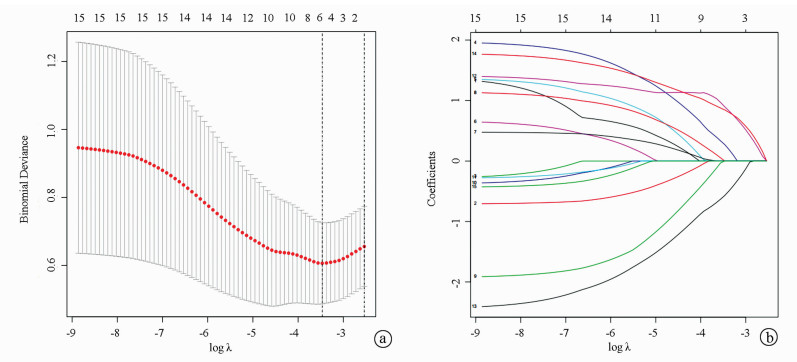
目的 对内镜微创保胆取石术后结石复发相关因素进行分析,根据独立危险因素,建立预测术后结石复发风险的列线图模型。 方法 回顾性分析2012年1月—2018年1月在青海大学附属医院接受内镜微创保胆取石术的144例胆囊结石患者的临床资料。根据术后结石复发情况将患者分为无复发组(n=130)和复发组(n=14)。两组间计数资料比较采用χ2检验。通过LASSO和logistic回归分析评价患者术后结石复发的独立风险因素,根据回归系数绘制相应的列线图预测模型。通过绘制校准曲线评估预测列线图的可靠性;采用Harrell一致性指数以量化预测列线图的判别性能;通过受试者工作特征曲线来评估该预测模型的灵敏度、特异度,计算曲线下面积(AUC)。 结果 144例患者内镜微创保胆取石术手术均获得成功,其中14例(9.7%)术后复发结石。通过多因素分析确定了4个影响复发的独立危险因素,分别为家族史(OR=3.245,95%CI:0.752~13.567,P=0.104)、饮食的规律性(OR=3.752,95%CI:1.067~14.141,P=0.041)、结石的均一性(OR=5.871,95%CI:1.636~25.390,P=0.010)和药物依从性(OR=0.225,95%CI:0.057~0.799,P=0.024)。列线图模型在建模样本中的一致性系数(C-index)为0.835(95%CI:0.732~0.938),在验证样本中的C-index为0.792 5,说明本研究列线图模型具有良好的精准度和区分度。预测列线图的AUC值为0.835,表明该列线图预测价值较高。 结论 家族史、饮食的规律性、胆结石的均一性和药物依从性是内镜微创保胆取石术后结石复发的独立危险因素,根据上述独立危险因素建立的列线图有助于预测术后结石复发的风险。 Abstract:Objective To investigate related factors for stone recurrence after endoscopic minimally invasive gallbladder-preserving cholecystolithotomy, and to establish a nomogram model for predicting the risk of stone recurrence after surgery based on independent risk factors. Methods A retrospective analysis was performed for the clinical data of 144 patients with gallstones who underwent endoscopic minimally invasive gallbladder-preserving cholecystolithotomy in Qinghai University Affiliated Hospital from January 2012 to January 2018, and according to postoperative stone recurrence, the patients were divided into non-recurrence group and recurrence group. The chi-square test was used for comparison of categorical data between two groups. LASSO and logistic regression analyses were used to analyze independent risk factors for postoperative stone recurrence, and the corresponding nomogram prediction model was plotted according to regression coefficient. The calibration curve was plotted to evaluate the reliability of the predictive nomogram; Harrell consistency index was used to quantify the discriminatory performance of the predictive nomogram; the receiver operating characteristic (ROC) curve was used to evaluate the sensitivity, specificity, and area under the ROC curve (AUC) of this predictive nomogram. Results All 144 patients underwent successful endoscopic minimally invasive gallbladder-preserving cholecystolithotomy, among whom 14 patients (9.7%) experienced stone recurrence after surgery. The multivariate analysis showed that family history (odds ratio [OR]= 3.245, 95% confidence interval [CI]: 0.752-13.567, P=0.104), regular diet (OR=3.752, 95% CI: 1.067-14.141, P=0.041), stone homogeneity (OR=5.871, 95% CI: 1.636-25.390, P=0.010), and medication compliance (OR=0.225, 95% CI: 0.057-0.799, P=0.024) were independent risk factors for recurrence. The nomogram model had an index of concordance (C-index) of 0.835 (95% CI: 0.732-0.938) in the modeling sample and 0.7925 in the verification sample, suggesting that the nomogram model in this study had good accuracy and discrimination. The predictive nomogram had an AUC of 0.835, suggesting that this nomogram had a relatively high predictive value. Conclusion Family history, regular diet, stone homogeneity, and medication compliance are independent risk factors for stone recurrence after endoscopic minimally invasive gallbladder-preserving cholecystolithotomy, and the nomogram constructed based on these independent risk factors may help to predict the risk of postoperative stone recurrence. -
Key words:
- Cholecystolithiasis /
- Recurrence /
- Nomograms
-
表 1 无复发组和复发组患者的基线特征
指标 无复发(n=130) 复发(n=14) 合计(n=144) χ2值 P值 年龄[例(%)] 2.695 0.747 ≤20岁 10(7.69) 2(14.29) 12(8.33) 21~30岁 27(20.77) 3(21.43) 30(20.83) 31~40岁 39(30.00) 3(21.43) 42(29.17) 41~50岁 42(32.31) 6(42.86) 48(33.33) 51~60岁 10(7.69) 0 10(6.95) >60岁 2(1.54) 0 2(1.39) 性别[例(%)] 0.106 0.745 女 82(63.08) 10(71.43) 92(63.89) 男 48(36.92) 4(28.57) 52(36.11) BMI[例(%)] 2.448 0.294 <24 kg/m2 85(65.38) 9(64.28) 94(65.28) 24~28 kg/m2 33(25.39) 2(14.29) 35(24.30) ≥28 kg/m2 12(9.23) 3(21.43) 15(10.42) 家族史[例(%)] 2.080 0.149 无 109(83.85) 9(64.29) 118(81.94) 有 21(16.15) 5(35.71) 26(18.06) 孕史[例(%)] 1.529 0.676 男性 48(36.92) 4(28.57) 52(36.11) 未孕 26(20.00) 3(21.43) 29(20.14) 孕1 42(32.31) 4(28.57) 46(31.94) 孕≥2 14(10.77) 3(21.43) 17(11.81) 饮食的规律性[例(%)] 8.386 0.004 规律 99(76.15) 5(35.71) 104(72.22) 不规律 31(23.85) 9(64.29) 40(27.78) 胆结石的数量[例(%)] 6.952 0.073 1个 81(62.31) 5(35.71) 86(59.72) 2个 17(13.08) 1(7.14) 18(12.50) 3个 6(4.61) 2(14.29) 8(5.56) >3个 26(20.00) 6(42.86) 32(22.22) 结石最大直径[例(%)] 3.857 0.145 <2 cm 86(66.15) 6(42.86) 92(63.89) 2 cm 33(25.39) 7(50.00) 40(27.78) ≥3 cm 11(8.46) 1(7.14) 12(8.33) 胆结石的均一性[例(%)] 7.906 0.005 均一 91(70.00) 4(28.57) 95(65.97) 不均一 39(30.00) 10(71.43) 49(34.03) 胆囊壁厚度[例(%)] 0.668 0.413 正常 93(71.54) 12(85.71) 105(72.92) 增厚 37(28.46) 2(14.29) 39(27.08) 胆囊黏膜光滑程度[例(%)] 0.000 0.999 光滑 101(77.69) 11(78.57) 112(77.78) 粗糙 29(22.31) 3(21.43) 32(22.22) 胆囊收缩功能[例(%)] 0.163 0.686 <30% 104(80.00) 10(71.43) 114(79.17) ≥30% 26(20.00) 4(28.57) 30(20.83) 术前TCH[例(%)] 0.045 0.832 <5.17 mmol/L 113(86.92) 13(92.86) 126(87.50) ≥5.17 mmol/L 17(13.08) 1(7.14) 18(12.50) 术前TG[例(%)] 0.000 0.999 <1.7 mmol/L 98(75.38) 11(78.57) 109(75.69) ≥1.7 mmol/L 32(24.62) 3(21.43) 35(24.31) 药物依从性[例(%)] 3.872 0.049 不规律 36(27.69) 8(57.14) 44(30.56) 规律 94(72.31) 6(42.86) 100(69.44) 表 2 内镜微创保胆取石术后复发的危险因素logistic回归结果
截距和变量 β值 OR(95%CI) P值 截距 -3.114 7 0.044(0.009~0.148) <0.001 家族史 1.177 1 3.245(0.752~13.567) 0.104 饮食的规律性 1.322 3 3.752(1.067~14.141) 0.041 胆结石的均一性 1.770 1 5.871(1.636~25.390) 0.010 药物依从性 -1.493 0 0.225(0.057~0.799) 0.024 -
[1] HE XY, SHI J. Consensus opinion on medical treatment of chronic cholecystitis and cholecystolithiasis in China (2018)[J]. J Clin Hepatol, 2019, 35(6): 1231-1236. (in Chinese) DOI: 10.3969/j.issn.1001-5256.2015.01.002何相宜, 施健. 中国慢性胆囊炎、胆囊结石内科诊疗共识意见(2018年)[J]. 临床肝胆病杂志, 2019, 35(6): 1231-1236. DOI: 10.3969/j.issn.1001-5256.2015.01.002 [2] KERLAN RK, LABERGE JM, RING EJ. Percutaneous cholecystolithotomy: Preliminary experience[J]. J Radiology, 1985, 157(3): 653-656. DOI: 10.1148/radiology.157.3.4059554 [3] CHESLYN-CURTIS S, RUSSELL RCG. Percutaneous cholecystolithotomy[J]. BMJ Clin Res, 1990, 301(6747): 339-340. [4] LIEVENS M, SCHUTZ SM. Percutaneous cholecystolithotomy: Is gall stone recurrence inevitable?[J]. Gastrointest Endosc, 1995, 41(3): 271-272. http://europepmc.org/articles/PMC1374759 [5] TAN YY, ZHAO G, WANG D, et al. A new strategy of minimally invasive surgery for cholecystolithiasis: Calculi removal and gallbladder preservation[J]. Dig Surg, 2013, 30(4-6): 466-471. DOI: 10.1159/000357823 [6] GAO DK, WEI SH, LI W, et al. Totally laparoscopic gallbladder-preserving surgery: A minimally invasive and favorable approach for cholelithiasis[J]. Exp Ther Med, 2015, 9(2): 395-398. DOI: 10.3892/etm.2014.2107 [7] SAUERBREI W, ROYSTON P, BINDER H. Selection of important variables and determination of functional form for continuous predictors in multivariable model building[J]. Stat Med, 2007, 26(30): 5512-5528. DOI: 10.1002/sim.3148 [8] FRIEDMAN J, HASTIE T, TIBSHIRANI R. Regularization paths for generalized linear models via coordinate descent[J]. J Stat Softw, 2010, 33(1): 1-22. http://neuro-oncology.oxfordjournals.org/external-ref?access_num=20808728&link_type=MED [9] KIDD AC, MCGETTRICK M, TSIM S, et al. Survival prediction in mesothelioma using a scalable Lasso regression model: Instructions for use and initial performance using clinical predictors[J]. BMJ Open Respir Res, 2018, 5(1): e000240. DOI: 10.1136/bmjresp-2017-000240 [10] BALACHANDRAN VP, GONEN M, SMITH JJ, et al. Nomograms in oncology: More than meets the eye[J]. Lancet Oncol, 2015, 16(4): e173-e180. DOI: 10.1016/S1470-2045(14)71116-7 [11] IASONOS A, SCHRAG D, RAJ GV, et al. How to build and interpret a nomogram for cancer prognosis[J]. J Clin Oncol, 2008, 26(8): 1364-1370. DOI: 10.1200/JCO.2007.12.9791 [12] KRAMER AA, ZIMMERMAN JE. Assessing the calibration of mortality benchmarks in critical care: The Hosmer-Lemeshow test revisited[J]. Crit Care Med, 2007, 35(9): 2052-2056. DOI: 10.1097/01.CCM.0000275267.64078.B0 [13] PENCINA MJ, D'AGOSTINO RB. Overall C as a measure of discrimination in survival analysis: Model specific population value and confidence interval estimation[J]. Stat Med, 2004, 23(13): 2109-2123. DOI: 10.1002/sim.1802 [14] ANDREW JV, ANGEL MC, ELENA BE, et al. Extensions to decision curve analysis, a novel method for evaluating diagnostic tests, prediction models and molecular markers[J]. BMC Medical Informatics and Decision Making, 2008, 8(15): 1039-1052. http://www.bmj.com/lookup/external-ref?access_num=10.1186/1472-6947-8-53&link_type=DOI [15] Development and validation of a radiomics nomogram for preoperative prediction of lymph node metastasis in colorectal cancer[J]. Science Foundation in China, 2016, 24(4): 35. [16] HAN XM, SHU XC, WANG YP. Research progress on the correlation between cholecystolithiasis, cholecystectomy and gastric cancer[J]. Med Rev, 2020, 26(13): 2559-2563, 2569. (in Chinese) https://www.cnki.com.cn/Article/CJFDTOTAL-YXZS202013013.htm韩雪梅, 舒小闯, 王玉平, 等. 胆囊结石及胆囊切除与胃癌相关性研究进展[J]. 医学综述, 2020, 26(13): 2559-2563, 2569. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZS202013013.htm [17] WEI L, CHAMPMAN S, LI X, et al. Beliefs about medicines and non-adherence in patients with stroke, diabetes mellitus and rheumatoid arthritis: A cross-sectional study in China[J]. BMJ Open, 2017, 7(10): e017293. DOI: 10.1136/bmjopen-2017-017293 [18] LI A, LIU JW, ZHANG D. Research progress on recurrence of cholecystolithiasis after endoscopic minimally invasive choledocholithiasis[J]. J Hepatopancreatobiliary Surg, 2019, 31(9): 573-577. (in Chinese) https://www.cnki.com.cn/Article/CJFDTOTAL-GDYW201909017.htm李骜, 刘江伟, 张东. 内镜微创保胆取石术后胆囊结石复发的研究进展[J]. 肝胆胰外科杂志, 2019, 31(9): 573-577. https://www.cnki.com.cn/Article/CJFDTOTAL-GDYW201909017.htm [19] CONDAT B, ZANDITENAS D, BARBU V, et al. Prevalence of low phospholipid-associated cholelithiasis in young female patients[J]. Dig Liver Dis, 2013, 45(11): 915-919. DOI: 10.1016/j.dld.2013.04.002 [20] GE HL, WAN H. Analysis of risk factors related to recurrence of gallstones after minimally invasive endoscopic choledocholithotomy[J]. J Binzhou Med Univ, 2016, 39(2): 149-150. (in Chinese) https://www.cnki.com.cn/Article/CJFDTOTAL-BZYB201602024.htm葛海龙, 万航. 微创内镜保胆取石术术后胆囊结石复发的相关危险因素分析[J]. 滨州医学院学报, 2016, 39(2): 149-150. https://www.cnki.com.cn/Article/CJFDTOTAL-BZYB201602024.htm [21] van de MEEBERG PC, PORTINCASA P, van de HEIJNING BJM, et al. Gallbladder (GB) emptying in vivo and contractility in vitro of gallstone patients on ursodeoxycholic acid(UDCA)[J]. Neth J Med, 1996, 48(1): A39. http://www.sciencedirect.com/science/article/pii/0300297796896458 [22] LIU T, LI N, LI D, et al. Clinical study on Xiaoshi Lidan capsule combined with ursodeoxycholic acid in the treatment of cholecystolithiasis[J]. China Pharm, 2019, 28(8): 30-32. (in Chinese) https://www.cnki.com.cn/Article/CJFDTOTAL-YYGZ201908013.htm刘彤, 李楠, 李栋, 等. 消石利胆胶囊联合熊去氧胆酸治疗胆囊结石临床研究[J]. 中国药业, 2019, 28(8): 30-32. https://www.cnki.com.cn/Article/CJFDTOTAL-YYGZ201908013.htm -



 PDF下载 ( 2761 KB)
PDF下载 ( 2761 KB)

 下载:
下载: