GLIM标准下3种营养筛查工具对肝硬化患者的适用性分析
DOI: 10.3969/j.issn.1001-5256.2022.02.019
Applicability of three nutritional screening tools in patients with liver cirrhosis under the Global Leadership Initiative on Malnutrition criteria
-
摘要:
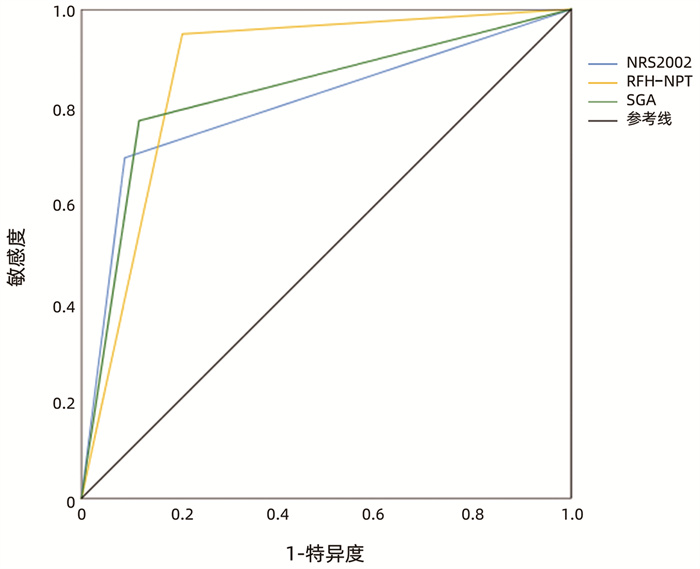
目的 探讨皇家自由医院-营养优先排序工具(RFH-NPT)与营养风险筛查2002(NRS2002)哪项更适合肝硬化患者的营养风险筛查,探讨主观全面营养评定(SGA)在肝硬化患者营养评估中的适用性。 方法 选取2020年8月—2021年6月在武汉大学人民医院住院的113例肝硬化患者,应用RFH-NPT和NRS2002进行营养风险筛查,应用SGA进行营养评估,将结果与全球(营养)领导层倡议营养不良(GLIM)诊断标准进行比较,分别计算出3种工具的敏感度、特异度、阳性预测值(PPV)、阴性预测值(NPV)。分别绘制3种筛查工具的受试者工作特征曲线(ROC曲线),并计算曲线下面积(AUC)。分析患者营养状况与短期预后的关系。计量资料两组间比较采用独立样本t检验或Mann-Whitney U检验,计数资料两组间比较采用χ2检验。NRS2002、RFHNPT、SGA与GLIM标准的相关性采用Spearman秩相关进行分析。 结果 GLIM标准下有69.9%的患者被诊断为营养不良,RFH-NPT和NRS2002分别筛查出72.6%和51.3%的患者存在营养风险,SGA评估下有57.5%的患者为营养不良。与NRS2002相比,RFH-NPT与GLIM标准具有更高的相关性(r=0.764,P<0.001),更高的敏感度(94.9%)和NPV(87.1%),且具有更好的预测价值(AUC=0.872,95%CI:0.786~0.957)。GLIM标准下,SGA诊断肝硬化患者营养不良的特异度较高(88.2%),敏感度一般(77.2%),具有良好的相关性(r=0.607,P<0.001)和预测价值(AUC=0.827,95%CI:0.744~0.911)。GLIM标准、SGA、RFH-NPT评估下,营养风险或营养不良患者的住院时间更长(Z值分别为-3.301、-2.812、-3.813,P值均<0.05),再住院率更高(χ2值分别为3.957、6.922、6.766,P值均<0.05)。GLIM标准、NRS2002评估下有营养风险或营养不良的患者3个月内病死率明显增加(χ2值分别为4.511、0.776,P值均<0.05)。 结论 GLIM标准下,RFH-NPT比NRS2002更适合肝硬化患者的营养风险筛查,SGA在肝硬化患者的营养评估中具有较好的适用性。此外,GLIM标准、SGA、RFH-NPT分别与患者的临床结局相关。 -
关键词:
- 肝硬化 /
- 营养不良 /
- 皇家自由医院-营养优先排序工具 /
- 营养风险筛查2002 /
- 主观全面营养评定
Abstract:Objective To investigate whether Royal Free Hospital Nutritional Prioritizing Tool (RFH-NPT) is more suitable than Nutritional Risk Screening 2002 (NRS-2002) in nutritional risk screening for patients with liver cirrhosis, as well as the applicability of subjective global assessment (SGA) in the nutritional assessment of patients with liver cirrhosis. Methods A total of 113 patients with liver cirrhosis who were hospitalized in Renmin Hospital of Wuhan University from August 2020 to June 2021 were enrolled. RFH-NPT and NRS-2002 were used for nutritional risk screening, and SGA was used for nutritional assessment. The results of these tools were compared with the Global Leadership Initiative on Malnutrition (GLIM) criteria, and sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) were calculated for the three tools. The receiver operating characteristic (ROC) curve was plotted and the area under the ROC curve (AUC) was calculated for each screening tool, and the association between nutritional status and short-term prognosis was analyzed. The independent samples t-test or the Mann-Whitney U test was used for comparison of continuous data between two groups, and the chi-square test was used for comparison of categorical data between two groups. The Spearman correlation analysis was used to analyze the correlation of GLIM criteria with NRS2002, RFH-NPT and SGA. Results According to the GLIM criteria, 69.9% of the patients were diagnosed with malnutrition, and RFH-NPT and NRS2002 screened out that 72.6% and 51.3%, respectively, of the patients had nutritional risk, while SGA assessment showed that 57.5% of the patients had malnutrition. Compared with NRS2002, RFH-NPT had a higher degree of correlation with the GLIM criteria (r=0.764, P < 0.001), higher sensitivity (94.9%) and NPV (87.1%), and a better predictive value (AUC=0.872, 95% confidence interval [CI]: 0.786-0.957). Under the GLIM criteria, SGA had good specificity (88.2%) in the diagnosis of malnutrition in patients with liver cirrhosis, with fair sensitivity (77.2%), good correlation (r=0.607, P < 0.001), and good predictive value (AUC=0.827, 95%CI: 0.744-0.911). Based on the GLIM criteria, SGA assessment, and RFH-NPT assessment, the patients with nutritional risk or malnutrition tended to have a longer length of hospital stay (Z=-3.301, -2.812, and -3.813, all P < 0.05) and a higher rehospitalization rate (χ2=3.957, 6.922, and 6.766, all P < 0.05). Based on the GLIM criteria and NRS2002 assessment, the patients with nutritional risk or malnutrition had a significant increase in mortality rate within 3 months (χ2=4.511 and 0.776, both P < 0.05). Conclusion Under the GLIM criteria, RFH-NPT is more suitable than NRS2002 for nutritional risk screening of patients with liver cirrhosis, and SGA also has good applicability in nutritional assessment of patients with liver cirrhosis. In addition, GLIM criteria, SGA, and RFH-NPT are associated with the clinical outcome of patients. -
Key words:
- Liver Cirrhosis /
- Malnutrition /
- RFH-NPT /
- NRS2002 /
- SGA
-
表 1 GLIM标准下肝硬化患者的基线特征及各临床指标与营养状况的关系
指标 总数(n=113) GLIM营养诊断 统计值 P值 营养良好(n=34) 营养不良(n=79) 年龄(岁) 56.81±10.90 52.09±9.47 58.84±10.90 t=-3.791 <0.001 男/女(例) 83/30 25/9 58/21 χ2=0.000 0.990 BMI(kg/m2) 20.80±3.44 23.34±2.74 19.7±3.13 t=6.400 <0.001 AMC(cm) 20.86(18.66~22.60) 22.73(21.99~23.25) 20.10(18.23~21.49) Z=-6.058 <0.001 MELD评分 10(8~13) 8(7~10) 11(8~15) Z=-3.859 <0.001 下肢水肿[例(%)] 22(19.5) 1(2.9) 21(26.6) χ2=8.473 <0.001 腹水[例(%)] 65(57.5) 5(14.7) 60(75.9) χ2=31.647 <0.001 肝性脑病[例(%)] 4(3.5) 1(2.9) 3(3.8) χ2=0.051 0.821 消化道出血[例(%)] 39(34.5) 14(41.2) 25(31.6) χ2=0.955 0.328 白蛋白(g/L) 33.67±6.62 38.51±5.10 31.58±6.10 t=5.581 <0.001 前白蛋白(g/L) 103.41±41.20 129.78±36.60 92.05±37.90 t=4.435 <0.001 总胆汁酸(μmol/L) 33.79(15.59~74.43) 24.71(9.97~41.33) 42.49(17.82~88.33) Z=-2.564 0.010 总胆红素(μmol/L) 20.80(14.44~37.70) 17.58(12.90~25.47) 22.60(14.54~46.07) Z=-2.035 0.016 胆碱酯酶(U/L) 3 598.0(2 678.5~5 293.5) 5 665.0(4 758.5~7 467.8) 3 038.0(2 361.0~4 038.0) Z=-5.083 <0.001 PT(s) 13.60(12.70~15.00) 12.85(11.78~13.70) 14.20(13.10~15.30) Z=-3.775 <0.001 INR 1.19(1.10~1.31) 1.12(1.02~1.19) 1.24(1.14~1.34) Z=-3.817 <0.001 表 2 不同营养评估方法下肝硬化患者营养风险及状况与肝功能分级关系
评估方法 Child-Pugh A级(n=60) Child-Pugh B级(n=39) Child-Pugh C级(n=14) χ2值 P值 NRS2002[例(%)] 23.766 <0.001 低风险 42(70.0) 12(30.7) 1(7.1) 中高风险 18(30.0) 27(69.3) 13(92.9) RFH-NPT[例(%)] 28.247 <0.001 低风险 29(48.3) 2(5.1) 0 中高风险 31(51.7) 37(94.9) 14(100) SGA[例(%)] 17.286 <0.001 营养良好 36(60.0) 11(28.2) 1(7.1) 中重度营养不良 24(40.0) 28(71.8) 13(92.9) GLIM[例(%)] 24.789 <0.001 营养良好 30(50.0) 4(10.3) 0 营养不良 30(50.0) 35(89.7) 14(100) 表 3 各营养筛查工具与GLIM标准下营养评定的相关性分析
评估方法 GLIM营养诊断[例] 敏感度(%) 特异度(%) PPV(%) NPV(%) r值 P值 营养良好(n=34) 营养不良(n=79) NRS2002 69.6 91.2 94.8 56.4 0.558 <0.001 低风险 31 24 中高风险 3 55 RFH-NPT 94.9 79.4 91.5 87.1 0.764 <0.001 低风险 27 4 中高风险 7 75 SGA 77.2 88.2 93.8 62.5 0.607 <0.001 营养良好 30 18 营养不良 4 61 表 4 不同评估方法下患者营养风险与短期预后的关系
预后指标 NRS2002 统计值 P值 RFH-NPT 统计值 P值 低风险(n=55) 中高风险(n=58) 低风险(n=31) 中高风险(n=82) 住院时间(d) 10(7~12) 12(9~15) Z=-1.268 0.205 8(7~11) 12(9~16) Z=-3.813 <0.001 3个月病死率[例(%)] 3(5.5) 12(20.7) χ2=0.776 0.017 1(3.2) 14(17.1) χ2=3.747 0.051 3个月再入院率[例(%)] 13(23.6) 18(31.0) χ2=5.692 0.378 3(9.7) 28(34.1) χ2=6.766 0.009 表 5 不同评估方法下患者营养状况与短期预后的关系
预后指标 SGA 统计值 P值 GLIM标准 统计值 P值 营养良好(n=48) 中重度营养不良(n=65) 营养良好(n=34) 营养不良(n=79) 住院时间(d) 10(7~12) 11(9~16) Z=-2.812 0.005 8(7~11) 12(9~15) Z=-3.301 0.001 3个月病死率[例(%)] 3(6.3) 12(16.9) χ2=3.576 0.059 1(2.9) 14(17.7) χ2=4.511 0.034 3个月再入院率[例(%)] 7(14.6) 24(36.9) χ2=6.922 0.009 5(14.7) 26(32.9) χ2=3.957 0.047 -
[1] KUFTINEC G, RAM BHAMIDIMARRI K, PEARLMAN M. Malnutrition in Cirrhosis: Frequent but overlooked[J]. Liver Transpl, 2019, 25(12): 1743-1744. DOI: 10.1002/lt.25660. [2] MAHARSHI S, SHARMA BC, SRIVASTAVA S. Malnutrition in cirrhosis increases morbidity and mortality[J]. J Gastroenterol Hepatol, 2015, 30(10): 1507-1513. DOI: 10.1111/jgh.12999. [3] SHIN S, JUN DW, SAEED WK, et al. A narrative review of malnutrition in chronic liver disease[J]. Ann Transl Med, 2021, 9(2): 172. DOI: 10.21037/atm-20-4868. [4] PLAUTH M, BERNAL W, DASARATHY S, et al. ESPEN guideline on clinical nutrition in liver disease[J]. Clin Nutr, 2019, 38(2): 485-521. DOI: 10.1016/j.clnu.2018.12.022. [5] BORHOFEN SM, GERNER C, LEHMANN J, et al. The royal free hospital-nutritional prioritizing tool is an independent predictor of deterioration of liver function and survival in cirrhosis[J]. Dig Dis Sci, 2016, 61(6): 1735-1743. DOI: 10.1007/s10620-015-4015-z. [6] ZHANG YH, YANG X, ZHANG D, et al. Application of subjective global nutritional assessment in patients with hepatitis-B-related liver cirrhosis[J]. Parenter Enteral Nutr, 2016, 23(6): 329-331. DOI: 10.16151/j.1007-810x.2016.06.0031.张颖慧, 杨雪, 张笛, 等. 主观综合性评估乙型肝炎性肝硬化病人的营养状况[J]. 肠外与肠内营养, 2016, 23(6): 329-331. DOI: 10.16151/j.1007-810x.2016.06.0031. [7] CEDERHOLM T, JENSEN GL, CORREIA M, et al. GLIM criteria for the diagnosis of malnutrition-A consensus report from the global clinical nutrition community[J]. J Cachexia Sarcopenia Muscle, 2019, 10(1): 207-217. DOI: 10.1002/jcsm.12383. [8] THEILLA M, RATTANACHAIWONG S, KAGAN I, et al. Validation of GLIM malnutrition criteria for diagnosis of malnutrition in ICU patients: An observational study[J]. Clin Nutr, 2021, 40(5): 3578-3584. DOI: 10.1016/j.clnu.2020.12.021. [9] HENRIQUE JR, PEREIRA RG, FERREIRA RS, et al. Pilot study GLIM criteria for categorization of a malnutrition diagnosis of patients undergoing elective gastrointestinal operations: A pilot study of applicability and validation[J]. Nutrition, 2020, 79-80: 110961. DOI: 10.1016/j.nut.2020.110961. [10] Chinese Society of Hepatology, Chinese Medical Association. Chinese guidelines on the management of liver cirrhosis[J]. J Clin Hepatol, 2019, 35(11): 2408-2425. DOI: 10.3969/j.issn.1001-5256.2019.11.006.中华医学会肝病学分会. 肝硬化诊治指南[J]. 临床肝胆病杂志, 2019, 35(11): 2408-2425. DOI: 10.3969/j.issn.1001-5256.2019.11.006. [11] European Association for the Study of the Liver. EASL clinical practice guidelines on nutrition in chronic liver disease[J]. J Hepatol, 2019, 70(1): 172-193. DOI: 10.1016/j.jhep.2018.06.024. [12] KONDRUP J, RASMUSSEN HH, HAMBERG O, et al. Nutritional risk screening (NRS 2002): A new method based on an analysis of controlled clinical trials[J]. Clin Nutr, 2003, 22(3): 321-336. DOI: 10.1016/s0261-5614(02)00214-5. [13] AMODIO P, BEMEUR C, BUTTERWORTH R, et al. The nutritional management of hepatic encephalopathy in patients with cirrhosis: International Society for Hepatic Encephalopathy and Nitrogen Metabolism Consensus[J]. Hepatology, 2013, 58(1): 325-336. DOI: 10.1002/hep.26370. [14] CIOCÎRLAN M, CAZAN AR, BARBU M, et al. Subjective global assessment and handgrip strength as predictive factors in patients with liver cirrhosis[J]. Gastroenterol Res Pract, 2017, 2017: 8348390. DOI: 10.1155/2017/8348390. [15] Chinese Society of Hepatology, Chinese Society of Gastroenterology, Chinese Medical Association. Clinical guidelines on nutrition in end-stage liver disease[J]. J Clin Hepatol, 2019, 35(6): 1222-1230. DOI: 10.3969/j.issn.1001-5256.2019.06.010.中华医学会肝病学分会, 中华医学会消化病学分会. 终末期肝病临床营养指南[J]. 临床肝胆病杂志, 2019, 35(6): 1222-1230. DOI: 10.3969/j.issn.1001-5256.2019.06.010. [16] BUCHARD B, BOIRIE Y, CASSAGNES L, et al. Assessment of malnutrition, sarcopenia and frailty in patients with cirrhosis: Which tools should we use in clinical practice?[J]. Nutrients, 2020, 12(1): 186. DOI: 10.3390/nu12010186. [17] ZHANG X, TANG M, ZHANG Q, et al. The GLIM criteria as an effective tool for nutrition assessment and survival prediction in older adult cancer patients[J]. Clin Nutr, 2021, 40(3): 1224-1232. DOI: 10.1016/j.clnu.2020.08.004. [18] KOOTAKA Y, KAMIYA K, HAMAZAKI N, et al. The GLIM criteria for defining malnutrition can predict physical function and prognosis in patients with cardiovascular disease[J]. Clin Nutr, 2021, 40(1): 146-152. DOI: 10.1016/j.clnu.2020.04.038. [19] BOULHOSA R, LOURENÇO RP, CÔRTES DM, et al. Comparison between criteria for diagnosing malnutrition in patients with advanced chronic liver disease: GLIM group proposal versus different nutritional screening tools[J]. J Hum Nutr Diet, 2020, 33(6): 862-868. DOI: 10.1111/jhn.12759. [20] BOJKO M. Causes of sarcopenia in liver cirrhosis[J]. Clin Liver Dis (Hoboken), 2019, 14(5): 167-170. DOI: 10.1002/cld.851. [21] ZHANG XN, JIANG ZM, WU HS, et al. NRS 2002 nutritional risk screening and GLIM step 2 for diagnosis of malnutrition (without FFMI currently)[J]. Chin J Clin Nutr, 2020, 28(1): 1-6. DOI: 10.3760/cma.j.cn115822-20190923-00141.张献娜, 蒋朱明, 吴河水, 等. NRS2002营养风险筛查暨GLIM第二步诊断营养不良(目前不用肌肉量理由)[J]. 中华临床营养杂志, 2020, 28(1): 1-6. DOI: 10.3760/cma.j.cn115822-20190923-00141. [22] SINCLAIR M. Controversies in diagnosing sarcopenia in cirrhosis-moving from research to clinical practice[J]. Nutrients, 2019, 11(10): 2454. DOI: 10.3390/nu11102454. [23] GUO Y, TANG ZQ. Progress on the application of detection and assessment tools for deficiency of liver cirrhosis[J/CD]. Chin J Liver Dis (Electronic Version), 2020, 12(1): 1-5. DOI: 10.3969/j.issn.1674-7380.2020.01.001.郭艳, 唐中权. 肝硬化营养不良检测手段与评估工具应用进展[J/CD]. 中国肝脏病杂志(电子版), 2020, 12(1): 1-5. DOI: 10.3969/j.issn.1674-7380.2020.01.001. [24] TRAUB J, BERGHEIM I, HORVATH A, et al. Validation of malnutrition screening tools in liver cirrhosis[J]. Nutrients, 2020, 12(5): 1306. DOI: 10.3390/nu12051306. [25] WU Y, ZHU Y, FENG Y, et al. Royal Free Hospital-Nutritional Prioritizing Tool improves the prediction of malnutrition risk outcomes in liver cirrhosis patients compared with Nutritional Risk Screening 2002[J]. Br J Nutr, 2020, 124(12): 1293-1302. DOI: 10.1017/S0007114520002366. [26] ALLARD JP, KELLER H, GRAMLICH L, et al. GLIM criteria has fair sensitivity and specificity for diagnosing malnutrition when using SGA as comparator[J]. Clin Nutr, 2020, 39(9): 2771-2777. DOI: 10.1016/j.clnu.2019.12.004. [27] MOCTEZUMA-VELAZQUEZ C, EBADI M, BHANJI RA, et al. Limited performance of subjective global assessment compared to computed tomography-determined sarcopenia in predicting adverse clinical outcomes in patients with cirrhosis[J]. Clin Nutr, 2019, 38(6): 2696-2703. DOI: 10.1016/j.clnu.2018.11.024. -



 PDF下载 ( 2135 KB)
PDF下载 ( 2135 KB)

 下载:
下载:


