基于内质网应激相关基因构建胰腺癌预后预测模型
DOI: 10.3969/j.issn.1001-5256.2023.12.021
伦理学声明:本研究方案于2022年2月28日经由吉林大学第一医院伦理委员会审批,批号:2022-017。
利益冲突声明:本文不存在任何利益冲突。
作者贡献声明:吕胜男负责课题设计,数据收集与分析,实验设计及操作,撰写论文;彭新宇负责数据分析及撰写代码;张健负责修改文章;刘欢负责组织样本收集及处理;魏锋负责拟定研究思路,指导文章撰写并最后定稿。
Establishment of a prognostic prediction model for pancreatic cancer based on endoplasmic reticulum stress-related genes
-
摘要:
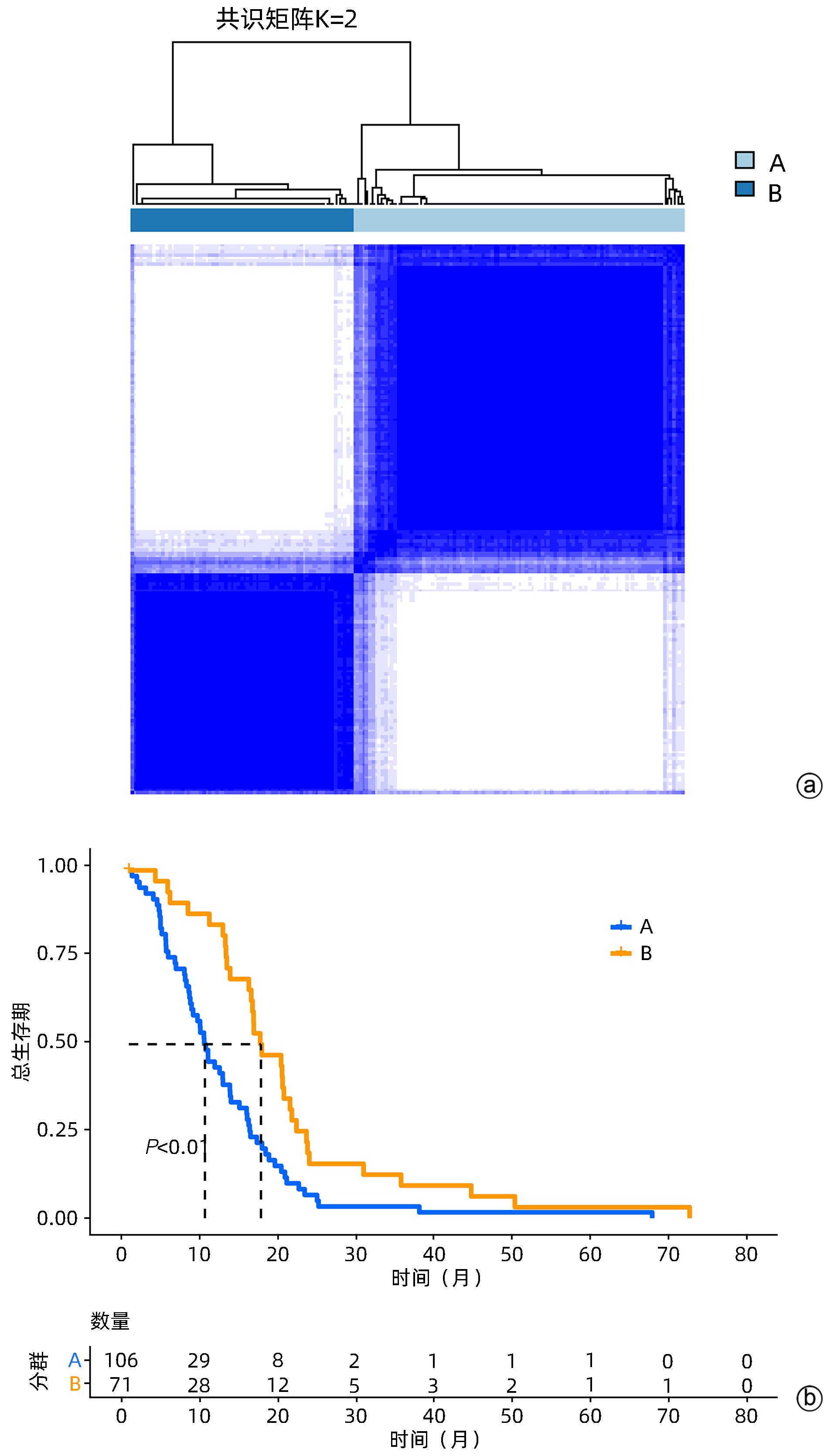
目的 阐明内质网应激基因在胰腺癌预后中的作用,寻找胰腺癌的预后标志物并构建预后预测模型。 方法 从TCGA和GTEx数据库下载转录组测序数据,通过MsigDB网站获取内质网应激基因,通过单因素Cox回归分析,获取预后相关基因,利用共识聚类分析方法构建胰腺癌分子分型,获取两亚群间的差异表达基因,通过Lasso回归分析,获得胰腺癌预后相关的核心基因,用于构建胰腺癌的预后预测模型,通过GEO数据库获取数据集对模型的预测性能进行验证。利用CIBERSORT分析风险评分与免疫浸润的相关性。实时荧光定量PCR检测基因在胰腺癌组织和细胞系中的表达情况。计量资料两组间比较采用成组t检验。计数资料两组间比较采用χ2检验。利用Log-rank检验进行生存期的比较。通过评估ROC曲线下的面积以评价模型的预测价值。 结果 内质网应激基因CEBPB、MARCKS、PMAIP1、UBXN10是胰腺癌预后的独立危险因素,基于它们的表达特征能够将TCGA胰腺癌队列分为两个亚群,簇A和簇B,簇A患者的总体生存期比簇B更短(χ2=12.232,P=0.01)。利用Lasso回归从簇A和簇B间差异表达的影响胰腺癌预后的基因中筛选出5个核心基因,获得的风险评分为:0.156×CDA+0.135×AHNAK2+0.020×RHOV+0.095×LY6D+0.054×SPRR1B,ROC曲线反映该模型的总体预测性能良好,1、3、5年的ROC曲线下面积分别为0.731、0.712、0.686,并且依据此模型划分的低风险组的总体生存期要长于高风险组(χ2=11.733,P=0.001)。该模型在外部数据集GSE57495中展现出了良好的预测性能。实时荧光定量PCR结果表明,与癌旁正常组织相比,CDA、AHNAK2、RHOV、LY6D、SPRR1B在40对胰腺癌组织中显著上调(t值分别为2.529、2.458、3.314、3.583、5.082,P值均<0.05)。 结论 根据CDA、AHNAK2、RHOV、LY6D、SPRR1B的表达特征可以预测胰腺癌预后,该组基因的整体高表达与胰腺癌患者的不良预后相关。 Abstract:Objective To investigate the role of endoplasmic reticulum stress genes in the prognosis of pancreatic cancer, and to establish a prognostic prediction model based on the prognostic markers for pancreatic cancer. Methods Transcriptome sequencing data were downloaded from TCGA and GTEx databases, and MsigDB website was used to obtain endoplasmic reticulum stress genes. A univariate Cox regression analysis was performed to obtain the genes associated with the prognosis of pancreatic cancer, and a consensus clustering analysis was used to construct the molecular typing of pancreatic cancer, while the differentially expressed genes between the two subgroups were obtained. A Lasso regression analysis was used to obtain the core genes associated with the prognosis of pancreatic cancer, which were used to construct a prognostic prediction model for pancreatic cancer. Related datasets were obtained from the GEO database to validate the predictive performance of the model. The CIBERSORT analysis was used to investigate the correlation between risk score and immune infiltration. Quantitative real-time PCR was used to measure the expression of genes in pancreatic cancer tissue and cell lines. The independent-samples t test was used for comparison of continuous data between two groups, and the chi-square test was used for comparison of categorical data between groups. Survival was compared using Log-rank test. The predictive value of the model was evaluated by evaluating the area under the ROC curve. Results The endoplasmic reticulum stress genes CEBPB, MARCKS, PMAIP1, and UBXN10 were independent risk factors for the prognosis of pancreatic cancer, and based on the expression characteristics of these genes, the TCGA pancreatic cancer cohort was divided into two subgroups, i.e., cluster A and cluster B, while the cluster A patients had a significantly shorter overall survival time than the cluster B patients (P<0.01). The Lasso regression analysis obtained 5 core genes from the differentially expressed genes affecting the prognosis of pancreatic cancer, and the risk scoring system was established as risk score=0.156×CDA+0.135×AHNAK2+0.020×RHOV+0.095×LY6D+0.054×SPRR1B. The ROC curve analysis showed that this model had good overall predictive performance, with the area under the ROC curve of 0.731 at 1 year, 0.712 at 3 years, and 0.686 at 5 years, and the low-risk group based on this model had a significantly longer overall survival time than the high-risk group (χ2=11.733, P=0.001). The model showed good predictive performance in the external dataset GSE57495. Quantitative real-time PCR results showed that the expression levels of CDA, AHNAK2, RHOV, LY6D, and SPRR1B in 40 pancreatic cancer tissue samples were significantly upregulated compared with those in normal adjacent tissue samples (t=2.529, 2.458, 3.314, 3.583, and 5.082, all P<0.05). Conclusion The expression characteristics of CDA, AHNAK2, RHOV, LY6D, and SPRR1B can be used to predict the prognosis of pancreatic cancer, and the high expression levels of these genes are associated with the poor prognosis of pancreatic cancer patients. -
Key words:
- Pancreatic Neoplasms /
- Endoplasmic Reticulum Stress /
- Prognosis /
- Risk Factors
-
表 1 引物序列
Table 1. Primer sequences
引物名称 引物序列(5'-3') CDA 上游引物:GCCAAGAAGTCAGCCTACTGCC 下游引物:CTTCTGGATAGCGGTCCGTTCA AHNAK2 上游引物:TCCTGGTGGAAGCGAGATTCAG 下游引物:ACCACCTGTGACACTGTAGCCA RHOV 上游引物:ACTGCGCTGGACACCTTCTCTG 下游引物:CACGCCAGGAAGACATCGGTAT LY6D 上游引物:AGCTCTCGCTTCTGCAAGACCA 下游引物:TCTCATTGCACAGGTCCTCCTG SPRR1B 上游引物:CTGCCCTTCAATAGTCACTCCAG 下游引物:CTCATACGCAGAATGGGATAGGG -
[1] SPRINGFELD C, FERRONE CR, KATZ MHG, et al. Neoadjuvant therapy for pancreatic cancer[J]. Nat Rev Clin Oncol, 2023, 20( 5): 318- 337. DOI: 10.1038/s41571-023-00746-1. [2] CUBILLOS-RUIZ JR, BETTIGOLE SE, GLIMCHER LH. Tumorigenic and immunosuppressive effects of endoplasmic reticulum stress in cancer[J]. Cell, 2017, 168( 4): 692- 706. DOI: 10.1016/j.cell.2016.12.004. [3] RAINES LN, ZHAO HX, WANG YZ, et al. PERK is a critical metabolic hub for immunosuppressive function in macrophages[J]. Nat Immunol, 2022, 23( 3): 431- 445. DOI: 10.1038/s41590-022-01145-x. [4] CHEN X, CUBILLOS-RUIZ JR. Endoplasmic reticulum stress signals in the tumour and its microenvironment[J]. Nat Rev Cancer, 2021, 21( 2): 71- 88. DOI: 10.1038/s41568-020-00312-2. [5] SAMANTA S, YANG SH, DEBNATH B, et al. The hydroxyquinoline analogue YUM70 inhibits GRP78 to induce ER stress-mediated apoptosis in pancreatic cancer[J]. Cancer Res, 2021, 81( 7): 1883- 1895. DOI: 10.1158/0008-5472.CAN-20-1540. [6] SIEGEL RL, MILLER KD, WAGLE NS, et al. Cancer statistics, 2023[J]. CA A Cancer J Clinicians, 2023, 73( 1): 17- 48. DOI: 10.3322/caac.21763. [7] WOOD LD, CANTO MI, JAFFEE EM, et al. Pancreatic cancer: Pathogenesis, screening, diagnosis, and treatment[J]. Gastroenterology, 2022, 163( 2): 386- 402.e1. DOI: 10.1053/j.gastro.2022.03.056. [8] CHANG XD, LI HY, CHEN J, et al. The role of lncRNA GAS5 in cell apoptosis, migration and invasion of AsPC-1 pancreatic cancer cell[J]. Clin J Med Offic, 2022, 50( 6): 599- 602. DOI: 10.16680/j.1671-3826.2022.06.15.常旭东, 李宏宇, 陈江, 等. 长链非编码RNA GAS5对胰腺癌AsPC-1细胞凋亡、迁移及侵袭能力调控作用[J]. 临床军医杂志, 2022, 50( 6): 599- 602. DOI: 10.16680/j.1671-3826. 2022.06.15. [9] TEMPERO MA. NCCN guidelines updates: Pancreatic cancer[J]. J Natl Compr Canc Netw, 2019, 17( 5.5): 603- 605. DOI: 10.6004/jnccn.2019.5007. [10] ZHANG TP, LIU YZ, REN B. Current status and challenges of total neoadjuvant therapy for pancreatic cancer[J]. Chin J Dig Surg, 2022, 21( 4): 461- 464. DOI: 10.3760/cma.j.cn115610-20220320-00141.张太平, 刘悦泽, 任博. 胰腺癌全程新辅助治疗的现状及挑战[J]. 中华消化外科杂志, 2022, 21( 4): 461- 464. DOI: 10.3760/cma.j.cn115610-20220320-00141. [11] CHEN BT, MAO XH. Clinical research advance in immunotherapy of pancreatic cancer[J]. Chin J Dig Surg, 2023, 22( 5): 610- 615. DOI: 10.3760/cma.j.cn115610-20230407-00158.陈博滔, 毛先海. 胰腺癌免疫治疗临床研究进展[J]. 中华消化外科杂志, 2023, 22( 5): 610- 615. DOI: 10.3760/cma.j.cn115610-20230407-00158. [12] LI ZX, GE Y, DONG J, et al. BZW1 facilitates glycolysis and promotes tumor growth in pancreatic ductal adenocarcinoma through potentiating eIF2α phosphorylation[J]. Gastroenterology, 2022, 162( 4): 1256- 1271.e14. DOI: 10.1053/j.gastro.2021.12.249. [13] ZHANG JF, YANG JY, LIN CY, et al. Endoplasmic reticulum stress-dependent expression of ERO1L promotes aerobic glycolysis in pancreatic cancer[J]. Theranostics, 2020, 10( 18): 8400- 8414. DOI: 10.7150/thno.45124. [14] LIU Z, LIU GL, HA DP, et al. ER chaperone GRP78/BiP translocates to the nucleus under stress and acts as a transcriptional regulator[J]. Proc Natl Acad Sci USA, 2023, 120( 31): e2303448120. DOI: 10.1073/pnas.2303448120. [15] NIU ZY, WANG MY, ZHOU L, et al. Elevated GRP78 expression is associated with poor prognosis in patients with pancreatic cancer[J]. Sci Rep, 2015, 5: 16067. DOI: 10.1038/srep16067. [16] MARTINEZ-USEROS J, GEORGIEV-HRISTOV T, BORRERO- PALACIOS A, et al. Identification of poor-outcome biliopancreatic carcinoma patients with two-marker signature based on ATF6α and p-p38 STARD compliant[J]. Medicine, 2015, 94( 45): e1972. DOI: 10.1097/MD.0000000000001972. [17] VANDE VOORDE J, SABUNCUOĞLU S, NOPPEN S, et al. Nucleoside-catabolizing enzymes in mycoplasma-infected tumor cell cultures compromise the cytostatic activity of the anticancer drug gemcitabine[J]. J Biol Chem, 2014, 289( 19): 13054- 13065. DOI: 10.1074/jbc.M114.558924. [18] GELLER LT, BARZILY-ROKNI M, DANINO T, et al. Potential role of intratumor bacteria in mediating tumor resistance to the chemotherapeutic drug gemcitabine[J]. Science, 2017, 357( 6356): 1156- 1160. DOI: 10.1126/science.aah5043. [19] LU D, WANG JX, SHI XY, et al. AHNAK2 is a potential prognostic biomarker in patients with PDAC[J]. Oncotarget, 2017, 8( 19): 31775- 31784. DOI: 10.18632/oncotarget.15990. [20] WANG XT, DOU XL, REN XX, et al. A ductal-cell-related risk model integrating single-cell and bulk sequencing data predicts the prognosis of patients with pancreatic adenocarcinoma[J]. Front Genet, 2021, 12: 763636. DOI: 10.3389/fgene.2021.763636. [21] LIU Y, SHAO ML, WU Y, et al. Role for the endoplasmic reticulum stress sensor IRE1alpha in liver regenerative responses[J]. J Hepatol, 2015, 62( 3): 590- 598. DOI: 10.1016/j.jhep.2014.10.022. -
 基于内质网应激相关基因构建胰腺癌预后预测模型.pdf
基于内质网应激相关基因构建胰腺癌预后预测模型.pdf

-



 PDF下载 ( 1296 KB)
PDF下载 ( 1296 KB)


 下载:
下载: